The Year 2000 Position Statement and Guidelines were developed by the Joint Committee on Infant Hearing (JCIH). Joint committee member organizations and their respective representatives who prepared this statement include (in alphabetical order) the American Academy of Audiology (Terese Finitzo, PhD, chair; and Yvonne Sininger, PhD); the American Academy of Otolaryngology–Head and Neck Surgery (Patrick Brookhouser, MD, vice-chair; and Stephen Epstein, MD); the American Academy of Pediatrics (Allen Erenberg, MD; and Nancy Roizen, MD); the American Speech-Language-Hearing Association (Allan O. Diefendorf, PhD; Judith S. Gravel, PhD; and Richard C. Folsom, PhD); the Council on Education of the Deaf whose member organizations include Alexander Graham Bell Association for the Deaf and Hard of Hearing, American Society for Deaf Children, Conference of Educational Administrators of Schools and Programs for the Deaf, Convention of American Instructors of the Deaf, National Association of the Deaf, and Association of College Educators of the Deaf and Hard of Hearing (Patrick Stone, EdD; Joseph J. Innes, PhD; and Donna M. Dickman, PhD*); and the Directors of Speech and Hearing Programs in State Health and Welfare Agencies (Lorraine Michel, PhD.; Linda Rose, MCD; and Thomas Mahoney, PhD). Ex officios to the JCIH include Evelyn Cherow, MA (American Speech-Language Hearing Association); Deborah Hayes, PhD (Marion Downs National Center for Infant Hearing); and Liz Osterhus, MA, and Thomas Tonniges, MD (American Academy of Pediatrics).
Joint committee member organizations that adopt this statement include (in alphabetical order) the American Academy of Audiology, the American Academy of Pediatrics, the American Speech-Language-Hearing Association (LC 7-2000), the Council on Education of the Deaf (see above individual organizations), and the Directors of Speech and Hearing Programs in State Health and Welfare Agencies.
*Donna Dickman, deceased.
Table of Contents
The Position Statement
I. Background
II. Principles
III. Guidelines for Early Hearing Detection and Intervention Programs
A. Roles and Responsibilities
1. Institutions and Agencies
2. Families and Professionals
B. Hearing Screening (Principles 1 and 8)
1. Personnel
2. Program Protocol Development
3. Screening Technologies
4. Screening Protocols
5. Benchmarks and Quality Indicators for Birth Admission Hearing Screening
C. Confirmation of Hearing Loss Referred From UNHS (Principles 2 and 8)
1. Audiologic Evaluation
2. Medical Evaluation
a. Pediatrician or Primary Care Physician
b. Otolaryngologist
c. Other medical specialists
3. Benchmarks and Quality Indicators for Confirmation of Hearing Loss
D. Early Intervention (Principles 3 and 8)
1. Early Intervention Program Development
2. Audiologic Habilitation
3. Medical and Surgical Intervention
4. Communication Assessment and Intervention
5. Benchmarks and Quality Indicators for Early Intervention Programs
E. Continued Surveillance of Infants and Toddlers (Principle 4)
1. Modification of the JCIH 1994 Risk Indicators
2. Risk indicators for use with neonates or infants
F. Protection of Infants' and Families' Rights (Principles 5 and 6)
G. Information Infrastructure (Principles 7 and 8) IV. Future Directions
References
The Position Statement
The Joint Committee on Infant Hearing (JCIH) endorses early detection of, and intervention for infants with hearing loss (early hearing detection and intervention, EHDI) through integrated, interdisciplinary state and national systems of universal newborn hearing screening, evaluation, and family-centered intervention. The goal of EHDI is to maximize linguistic and communicative competence and literacy development for children who are hard of hearing or deaf. Without appropriate opportunities to learn language, children who are hard of hearing or deaf will fall behind their hearing peers in language, cognition, and social-emotional development. Such delays may result in lower educational and employment levels in adulthood (Gallaudet University Center for Assessment and Demographic Study, 1998). Thus, all infants' hearing should be screened using objective, physiologic measures in order to identify those with congenital or neonatal onset hearing loss. Audiologic evaluation and medical evaluations should be in progress before 3 months of age. Infants with confirmed hearing loss should receive intervention before 6 months of age from health care and education professionals with expertise in hearing loss and deafness in infants and young children. Regardless of prior hearing screening outcomes, all infants who demonstrate risk indicators for delayed onset or progressive hearing loss should receive ongoing audiologic and medical monitoring for 3 years and at appropriate intervals thereafter to ensure prompt identification and intervention (American Speech-Language-Hearing Association, 1997). EHDI systems should guarantee seamless transitions for infants and their families through this process.
Appropriate early intervention programs are family-centered, interdisciplinary, culturally competent, and build on informed choice for families (Baker-Hawkins & Easterbrooks, 1994). To achieve informed decision making, families should have access to professional, educational, and consumer organizations, and they should have opportunities to interact with adults and children who are hard of hearing and deaf (Ogden, 1996; Thompson, 1994). Families should have access to general information on child development and specific information on hearing loss and language development. To achieve accountability, individual community and state, health and educational programs should assume the responsibility for coordinated, ongoing measurement and improvement of EHDI process outcomes.
I. Background
Hearing loss in newborns and infants is not readily detectable by routine clinical procedures (behavioral observation), although parents often report the suspicion of hearing loss, inattention, or erratic response to sound before hearing loss is confirmed (Arehart, Yoshinaga-Itano, Thomson, Gabbard, & Stredler Brown, 1998; Harrison & Roush, 1996; Kile, 1993). The average age of identification in the United States is being reduced with EHDI programs; until very recently, it had been 30 months of age (Harrison & Roush, 1996). Although children who have severe to profound hearing loss or multiple disabilities may be identified before 30 months, children with mild-to-moderate losses often are not identified until school age because of the nature of hearing loss and the resultant inconsistent response to sound (Elssmann, Matkin, & Sabo, 1987). For this reason, the National Institute on Deafness and Other Communication Disorders (of the National Institutes of Health) released a Consensus Statement on Early Identification of Hearing Impairment in Infants and Young Children in 1993. The statement concluded that all infants admitted to the neonatal intensive care unit (NICU) should be screened for hearing loss before hospital discharge and that universal screening should be implemented for all infants within the first 3 months of life (NIDCD, 1993). In its 1994 Position Statement, the JCIH endorsed the goal of universal detection of infants with hearing loss and encouraged continuing research and development to improve methodologies for identification of and intervention for hearing loss (Joint Committee on Infant Hearing, 1994a, 1994b, 1995a, 1995b).
In the ensuing years, considerable data have been reported that support not only the feasibility of universal newborn hearing screening (UNHS) but also the benefits of early intervention for infants with hearing loss (Moeller, in press). Specifically, infants who are hard of hearing and deaf who receive intervention before 6 months of age maintain language development commensurate with their cognitive abilities through the age of 5 years (Yoshinaga-Itano, 1995; Yoshinaga-Itano, Sedey, Coulter, & Mehl, 1998). Numerous investigators have documented the validity, reliability, and effectiveness of early detection of infants who are hard of hearing and deaf through universal newborn hearing screening (Finitzo, Albright, & O'Neal, 1998; Prieve and Stevens, 2000; Spivak, 1998; Spivak et al., 2000; Vohr, Carty, Moore, & Letourneau, 1998; Vohr & Maxon, 1996). Cost-effective screening is being undertaken in individual hospitals and in numerous statewide programs in the United States (Arehart, Yoshinaga-Itano, Thomson, Gabbard, & Stredler Brown, 1998; Finitzo, Albright, & O'Neal, 1998; Mason & Hermann, 1998; Mehl & Thomson, 1998; Vohr, Carty, Moore, & Letourneau, 1998). As of Spring 2000, more than half of the States have enacted legislation supporting universal newborn hearing screening. Working groups convened by the National Institute on Deafness and Other Communication Disorders (NIDCD) in 1997 and 1998 offered recommendations on Acceptable Protocols for Use in State-Wide Universal Newborn Hearing Screening Programs and Characterization of Auditory Performance and Intervention Strategies Following Neonatal Screening (NIDCD, 1997, 1998). Given these findings and empirical evidence to date, the JCIH considers that accepted public health criteria have been met to justify implementation of universal newborn hearing screening (American Academy of Pediatrics, 1999a,b; American Speech-Language-Hearing Association, 1989; Spivak, 1998). The JCIH issues the year 2000 Position Statement, describes principles underlying effective EHDI programs, and provides an accompanying guideline on implementing and maintaining a successful EHDI program.
II. Principles
The Joint Committee on Infant Hearing (JCIH) endorses the development of family-centered, community-based EHDI systems. EHDI systems are comprehensive, coordinated, timely, and available to all infants. The following eight principles provide the foundation for effective EHDI systems. Each of the principles is discussed in the Guideline, which follows the delineation of the principles.
1. All infants have access to hearing screening using a physiologic measure. Newborns who receive routine care have access to hearing screening during their hospital birth admission. Newborns in alternative birthing facilities, including home births, have access to and are referred for screening before 1 month of age. All newborns or infants who require neonatal intensive care receive hearing screening before discharge from the hospital. These components constitute universal newborn hearing screening (UNHS).
2. All infants who do not pass the birth admission screen and any subsequent rescreening begin appropriate audiologic and medical evaluations to confirm the presence of hearing loss before 3 months of age.
3. All infants with confirmed permanent hearing loss receive services before 6 months of age in interdisciplinary intervention programs that recognize and build on strengths, informed choice, traditions, and cultural beliefs of the family.
4. All infants who pass newborn hearing screening but who have risk indicators for other auditory disorders and/or speech and language delay receive ongoing audiologic and medical surveillance and monitoring for communication development. Infants with indicators associated with late-onset, progressive, or fluctuating hearing loss as well as auditory neural conduction disorders and/or brainstem auditory pathway dysfunction should be monitored.
5. Infant and family rights are guaranteed through informed choice, decision-making, and consent.
6. Infant hearing screening and evaluation results are afforded the same protection as all other health care and educational information. As new standards for privacy and confidentiality are proposed, they must balance the needs of society and the rights of the infant and family, without compromising the ability of health and education to provide care (AAP, 1999).
7. Information systems are used to measure and report the effectiveness of EHDI services. Although state registries measure and track screening, evaluation, and intervention outcomes for infants and their families, efforts should be made to honor a family's privacy by removing identifying information wherever possible. Aggregate state and national data may also be used to measure and track the impact of EHDI programs on public health and education while maintaining the confidentiality of individual infant and family information.
8. EHDI programs provide data to monitor quality, demonstrate compliance with legislation and regulations, determine fiscal accountability and cost effectiveness, support reimbursement for services, and mobilize and maintain community support.
III. Guidelines for Early Hearing Detection and Intervention Programs
These Guidelines are developed to supplement the eight JCIH Year 2000 Position Statement Principles and to support the goals of universal access to hearing screening, evaluation, and intervention for newborns and infants embodied in Healthy People 2000 (U.S. Department of Health and Human Services Public Health Service, 1990) and 2010 (U.S. Department of Health and Human Services, 2000). The Guidelines provide current information on the development and implementation of successful EHDI systems.
Hearing screening should identify infants at risk for specifically defined hearing loss that interferes with development. On the basis of investigations of long-term, developmental consequences of hearing loss in infants, current limitations of physiologic screening techniques, availability of effective intervention, and in concert with established principles of health screening (American Academy of Pediatrics, 1999b; Fletcher, Fletcher, & Wagner, 1988; Sackett, Haynes, & Tugwell, 1991), the JCIH defines the targeted hearing loss for UNHS programs as permanent bilateral or unilateral, sensory or conductive hearing loss, averaging 30 to 40 dB or more in the frequency region important for speech recognition (approximately 500 through 4000 Hz). The JCIH recommends that all infants with the targeted hearing loss be identified so that appropriate intervention and monitoring may be initiated.
Hearing loss as defined above has effects on communication, cognition, behavior, social-emotional development, and academic outcomes and later vocational opportunities (Karchmer & Allen, 1999). These effects have been well documented by large-scale research investigations in children with (a) mild-to-profound bilateral hearing loss (Bess & McConnell, 1981; Blair, Peterson, & Vieweg, 1985; Carney & Moeller, 1998; Davis, Elfenbein, Schum, & Bentler, 1986; Davis, Shepard, Stelmachowicz, & Gorga, 1981; Karchmer & Allen, 1999), (b) moderate-to-profound unilateral sensorineural hearing loss (Bess & Tharpe, 1984, 1986; Oyler, Oyler, & Matkin, 1988), and (c) minimal flat or sloping sensory hearing loss (Bess, Dodd-Murphy, & Parker, 1998). The incidence and/or prevalence of these types of hearing loss have also been described (Bess, Dodd-Murphy, & Parker, 1998; Dalzell et al., 2000; Finitzo, Albright, & O'Neal, 1998; Mehl & Thomson, 1998). For children with mild-to-profound bilateral sensory hearing loss, effective habilitation strategies including use of personal amplification, language development programs, and speech training have been described (Goldberg & Flexer, 1993; Stelmachowicz, 1999; Yoshinaga-Itano, Sedey, Coulter, & Mehl, 1998).
Depending on the screening technology selected, infants with hearing loss less than 30 dB HL or with hearing loss related to auditory neuropathy or neural conduction disorders may not be detected in a universal newborn hearing screening program. Although the JCIH recognizes that these disorders may result in developmental delay, limitations of some currently recommended screening technologies preclude cost-effective detection of these disorders. All infants, regardless of newborn hearing screening outcome, should receive ongoing monitoring for development of age-appropriate auditory behaviors and communication skills. Any infant who demonstrates delayed auditory and/or communication skills development should receive audiologic evaluation to rule out hearing loss.
The JCIH supports applying the concepts of continual process or quality improvement to each component of EHDI programs to achieve desired outcomes. The JCIH recommends that systems be designed to achieve quality outcomes for infants and their families and for hospital, state, and national programs. Specifically, at each step in the process of care, performance measures should be undertaken to examine whether the system conforms to accepted standards of quality (Finitzo, 1999; Tharpe & Clayton, 1997). This guideline outlines the benchmarks and associated quality indicators that serve to monitor compliance and outcomes at each step in the EHDI process.
Benchmarks are quantifiable goals or targets by which an EHDI program may be monitored and evaluated. Benchmarks are used to evaluate progress and to point to needed next steps in achieving and maintaining a quality EHDI program (O'Donnell & Galinsky, 1998). Because EHDI programs are relatively new, the JCIH has included examples of established benchmarks that are based on existing data and suggested benchmarks in areas where published data are not currently available. Quality indicators reflect a result in relation to a stated benchmark. Quality indicators should be monitored using well-established practices of statistical process control to determine program consistency and stability (Wheeler & Chambers, 1986). If the quality indicators demonstrate that a program is not meeting the stated benchmark, sources of variability should be identified and corrected to improve the process (Tharpe & Clayton, 1997). It is prudent for hospitals and state programs to establish a periodic review process to evaluate benchmarks as more data on EHDI outcomes become available and to examine how program quality indicators are conforming to established benchmarks.
A. Roles and Responsibilities
1. Institutions and Agencies. A variety of public and private institutions and agencies may assume responsibility for specific components (e.g., screening, evaluation, intervention) of a comprehensive EHDI program and the training required for EHDI success. State and local agencies that are involved in components of an EHDI program should work collaboratively to define their roles, responsibilities, and accountability. These roles and responsibilities may differ from state to state; however, it is strongly recommended that each state identify a lead coordinating agency with oversight responsibility for EHDI. The lead coordinating agency should convene an advisory committee consisting of professionals, families with children who are hard of hearing or deaf, members of the hard of hearing and Deaf communities, and other interested community leaders to provide guidance on the development, coordination, funding, and quality evaluation of community-based EHDI programs (ASHA, AAA, & AG Bell, 1997; Model Universal Newborn/Infant Hearing Screening, Tracking, and Intervention Bill). The lead coordinating agency in each state should be responsible for identifying the public and private funding sources available to support development, implementation, and coordination of EHDI systems. Funding sources may vary from year to year. Currently, federal sources of systems support include Title V block grants to states for maternal and child health care services, Title XIX (Medicaid) federal and state funds for eligible children, and competitive U.S. Department of Education demonstration and research grants. The National Institute on Deafness and Other Communication Disorders provides grants for research related to early identification and intervention for children who are hard of hearing and deaf. Sources of reimbursement for services to individual children will vary from state to state and may include private medical insurance coverage.
2. Families and Professionals. The success of EHDI programs depends on professionals working in partnership with families as a well-coordinated team (Moeller, in press). The roles and responsibilities of each team member should be well defined and clearly understood. Essential team members are families, pediatricians or primary care physicians, audiologists, otolaryngologists, speech-language pathologists, educators of children who are hard of hearing or deaf, and other early intervention professionals involved in delivering EHDI services (Joint Committee of ASHA and Council on Education of the Deaf, 1994). Provisions for supportive family education, counseling, and guidance should be available (Calderon, Bargones, & Sidman, 1998).
Pediatricians and other primary care physicians, working in partnership with parents and other health-care professionals, make up the infant's "medical home." A medical home is defined as an approach to providing health care services where care is accessible, family-centered, continuous, comprehensive, coordinated, compassionate, and culturally competent. Pediatricians act in partnership with parents in a medical home to identify and access services needed in developing a global plan of appropriate and necessary health and habilitative care for infants identified with hearing loss. The infant's pediatrician or other primary care physician functions as the advocate for the whole child within the context of the medical home (American Academy of Pediatrics, 1992, 1993).
As experts in identification, evaluation, and auditory habilitation of infants who are hard of hearing and deaf, audiologists are involved in each component of the EHDI process. For the hearing screening component, audiologists provide program development, management, quality assessment, service coordination, and effective transition to evaluation, habilitative, and intervention services. For the follow-up component, audiologists provide comprehensive audiologic assessment to confirm the existence of the hearing loss, evaluate the infant for candidacy for amplification and other sensory devices and assistive technology, and ensure prompt referral to early intervention programs. For the early intervention component, audiologists provide timely fitting and monitoring of amplification (sensory devices and assistive technology) with family consent, family education, counseling, and ongoing participation in the infant's service plan (Pediatric Working Group of the Conference on Amplification for Children with Auditory Deficits, 1996). In addition, audiologists provide direct auditory habilitation services to infants and families. Audiologists participate in the assessment of candidacy for cochlear implantation.
Otolaryngologists are physicians whose specialty includes the identification, evaluation, and treatment of ear diseases and syndromes related to hearing loss. Families consult an otolaryngologist to determine the etiology of the hearing loss, the presence of related syndromes involving the head and neck structures, and related risk indicators (Section III. E below) for hearing loss. An otolaryngologist with expertise in childhood hearing loss can determine whether medical and/or surgical intervention may be appropriate. When medical and/or surgical intervention is provided, the otolaryngologist is involved in the long-term monitoring and follow-up within the infant's medical home. The otolaryngologist also provides information and participates in the assessment for candidacy for amplification, assistive devices, and cochlear implantation.
Early intervention professionals provide comprehensive family-centered services. They are professionals trained in a variety of academic disciplines, such as speech-language pathology, audiology, education of children who are hard of hearing and deaf, service coordination, or early childhood special education. All individuals who provide services to infants with hearing loss should have training and expertise in auditory, speech, and language development; communication approaches for infants with hearing loss and their families (e.g., cued speech, sign language systems including American Sign Language); and child development (Ross, 1990; Stredler-Brown, 1999). Speech-language pathologists provide both evaluation and treatment for language, speech, and cognitive-communication development (ASHA, 1989). Educators of children who are hard of hearing and deaf integrate the development of communicative competence within the infant's entire development, including a variety of social, linguistic, and cognitive/academic contexts (Joint Committee of ASHA & CED, 1994). In collaboration with the family and other EHDI team members, the service coordinator (case manager) facilitates the family's transition from screening to evaluation to early intervention; links the family to the local Part C system (Public Law 105-17: the amendments to the Individuals with Disabilities Education Act, IDEA, 1997; U.S. Department of Education, Office of Special Education and Rehabilitative Services, 1998); monitors the timeliness of the services; and provides information regarding program options, funding sources, communication choices, and emotional support. This professional incorporates the family's preferences for outcomes into an individualized family service plan (IFSP) as required by federal legislation (IDEA, as defined above). The service coordinator supports the family in stimulation of the infant's communicative development; monitors the infant's progress in language, motor, cognitive and social-emotional development in the IFSP review; and assists the family in advocating for its infant's unique developmental needs.
B. Hearing Screening (Principles 1 and 8)
1. Personnel. Teams of professionals, including audiologists, physicians (neonatologists, pediatricians, other primary care physicians, and otolaryngologists), and nursing personnel, should be involved in establishing the UNHS component of EHDI programs. Hospitals and agencies should designate a physician to oversee the medical aspects of the EHDI program. Audiologists should be designated as the program manager with supervisory responsibilities for the hearing screening and audiologic aspects of the EHDI program and should be involved in the design, implementation, and evaluation of screening programs (including those of small and rural hospitals) (Joint Committee on Infant Hearing, 1994a,b). In addition to audiologists, personnel who carry out the screening procedure may include nurses, speech-language pathologists, and others who are trained by the audiologist (American Academy of Audiology, 1998; American Speech-Language-Hearing Association, 1997; National Institute on Deafness and Other Communication Disorders, 1993, 1997; White & Maxon, 1999).
2. Program Protocol Development. Each team of professionals responsible for the hospital-based UNHS program needs to undertake a comprehensive review of the current hospital infrastructure before implementation of screening. The development of a hospital-based screening program should consider technology, screening protocols including the timing of the screening relative to nursery discharge, availability of qualified screening personnel, acoustically appropriate environments, follow-up referral criteria, information management, and quality control. Reporting and communication management must all be defined. These include the content of reports to physicians and parents, documentation of results in medical records, and methods for reporting to state registries and national data sets. Methods for ensuring that communications to parents are confidential and sensitive should be well defined. Health communication specialists should work with EHDI stakeholders to develop and disseminate family information materials that are accessible and represent the range of alternatives. Materials should be produced in languages other than English for diverse cultures and for low-literacy consumers. Quality indicators and outcome measurements for each component of the UNHS program should be identified and defined before implementation of screening to monitor compliance with program benchmarks. Solutions to problems are often found at the local level. Community resources should be accessed to achieve successful implementation of UNHS.
3. Screening Technologies. Objective physiologic measures must be employed to detect newborns and very young infants with the targeted hearing loss. Current physiologic measures used for detecting unilateral or bilateral hearing loss of various severities include otoacoustic emissions (OAEs), either transient-evoked (TEOAE) or distortion-product (DPOAE), and/or auditory brainstem response (ABR). Both OAE and ABR technologies have been successfully implemented for universal newborn hearing screening (Finitzo, Albright, & O'Neal, 1998; Mason & Hermann, 1998; Vohr, Carty, Moore, & Letourneau, 1998). Both technologies are noninvasive recordings of physiologic activity that underlie normal auditory function and that are easily recorded in neonates. Both OAE and ABR measures are highly correlated with the degree of peripheral hearing sensitivity.
OAEs are sensitive to outer hair cell dysfunction. The technology can be used to detect sensory (i.e., inner ear) hearing loss (Gorga et al., 1993; Prieve et al., 1993). OAEs can be reliably recorded in neonates in response to stimuli in the frequency range above 1500 Hz. The OAE is known to be sensitive to outer ear canal obstruction and middle ear effusion, and, therefore, temporary conductive dysfunction can cause a positive test result (a "refer" outcome) in the presence of normal cochlear function (Doyle, Burggraaff, Fujikawa, Kim, & MacArthur, 1997). Because OAE responses are generated within the cochlea by the outer hair cells, OAE evaluation does not detect neural (i.e., eighth nerve or auditory brainstem pathway) dysfunction. Infants with auditory neuropathy or neural conduction disorders without concomitant sensory (i.e., outer hair cell) dysfunction will not be detected by OAEs.
The ABR reflects activity of the cochlea, auditory nerve, and auditory brainstem pathways. When used as a threshold measure, the click-evoked ABR is highly correlated with hearing sensitivity in the frequency range from 1000 to 8000 Hz (Gorga et al., 1993; Hyde, Riko, & Malizia, 1990). The ABR is sensitive to auditory nerve and brainstem dysfunction; therefore, ABR screening may result in a positive test (a "refer" outcome) in the absence of peripheral (e.g., middle ear or cochlear) hearing loss. Because the ABR is generated by auditory neural pathways, the ABR will detect auditory neuropathy or neural conduction disorders in newborns.
Development of a program includes the establishment of the interpretive criteria for pass and refer. Interpretive criteria should be founded on a clear scientific rationale. Such rationale may be based in statistics and signal detection theory or heuristic and empirically derived. Test performance efficiency, including sensitivity, specificity, and the positive and negative predictive values, should be evidenced-based (Hyde, Davidson, & Alberti, 1991; Hyde, Sininger, & Don, 1998). Screening technologies that incorporate automated response detection are preferred over those that require operator interpretation and decision making. Automated algorithms eliminate the need for individual test interpretation, reduce the effects of screener bias and errors on test outcome, and ensure test consistency across all infants, test conditions, and screening personnel (Eilers, Miskiel, Ozdamar, Urbano, & Widen, 1991; Herrmann, Thornton, & Joseph, 1995; McFarland, Simmons, & Jones, 1980; Ozdamar, Delgado, Eilers, & Urbano, 1994; Pool & Finitzo, 1989). Programs that use trained and supervised nonprofessional staff must use technologies that provide automated pass-refer criteria. Before incorporating automated response detection algorithms, however, the screening program must ensure that the algorithms have been validated by rigorous scientific methods and that those results have been reported in peer-reviewed publications.
Some infants with hearing loss will pass the newborn hearing screening. Both ABR and OAE technology can show false-negative findings, depending on whether hearing loss exists in configurations that include normal hearing for one or more frequencies in the target range. These would include isolated low-frequency (i.e., below 1000 Hz) hearing loss or steeply sloping high-frequency (i.e., above 2000 Hz) hearing loss. ABR can show false-negative findings with midfrequency hearing loss (i.e., 500-2000 Hz). Additional variables that influence screening test performance include the population (age and presence of risk indicators), the targeted hearing loss, the performance and recording characteristics of the test technology, the pass-refer criteria, and excessive retesting using the same technology (which increases the likelihood of a false-negative screening outcome).
4. Screening Protocols. A variety of hospital-based UNHS screening protocols have been successfully implemented that permit all newborns access to hearing screening during their birth admission (Arehart, Yoshinaga-Itano, Thomson, V., Gabbard, & Stredler Brown, 1998; Finitzo, Albright, & O'Neal, 1998; Gravel et al., 2000; Mason & Hermann, 1998; Mehl & Thomson, 1998; Vohr, Carty, Moore, & Letourneau, 1998). Most infants pass their initial screening test. Many inpatient-screening protocols provide one or more repeat screens, using the same or a different technology, if the newborn does not pass the initial birth screen. For example, hospitals may screen with OAE technology or ABR technology and retest infants who "refer" with the same or the other technology.
Some screening protocols incorporate an outpatient rescreening of infants who do not pass the birth admission screening within 1 month of hospital discharge. The mechanism of rescreening an infant minimizes the number of false-positive referrals for follow-up audiologic and medical evaluation. Outpatient screening by 1 month of age should also be available to infants who were discharged before receiving the birth admission screening or who were born outside a hospital or birthing center.
5. Benchmarks and Quality Indicators for Birth Admission Hearing Screening.
(a) Recommended UNHS benchmarks include the following:
(1) Within 6 months of program initiation, hospitals or birthing centers screen a minimum of 95% of infants during their birth admission or before 1 month of age. Programs can achieve and maintain this outcome despite birth admissions of 24 or fewer hours (Finitzo, Albright, & O'Neal, 1998; Mason & Hermann, 1998; Spivak et al., 2000; Vohr, Carty, Moore, & Letourneau, 1998).
(2) The referral rate for audiologic and medical evaluation following the screening process (in-hospital during birth admission or during both birth admission and outpatient follow-up screening) should be 4% or less within 1 year of program initiation.
(3) The agency within the EHDI program with defined responsibility for follow-up (often a state department of health) documents efforts to obtain follow-up on a minimum of 95% of infants who do not pass the hearing screening. Ideally, a program should achieve a return-for-follow-up of 70% of infants or more (Prieve et al., 2000). Successful follow-up is influenced by such factors as lack of adequate tracking information, changes in the names or addresses of mother and/or infant, absence of a designated medical home for the infant, and lack of health insurance that covers follow-up services.
(b) Associated quality indicators of the screening component of EHDI programs may include the following:
(1) Percentage of infants screened during the birth admission.
(2) Percentage of infants screened before 1 month of age.
(3) Percentage of infants who do not pass the birth admission screen.
(4) Percentage of infants who do not pass the birth admission screening who return for follow-up services (either outpatient screening and/or audiologic and medical evaluation).
(5) Percentage of infants who do not pass the birth admission/outpatient screen(s) who are referred for audiologic and medical evaluation.
(6) Percentage of families who refuse hearing screening on birth admission.
Quality indicators for hospital-based programs should be monitored monthly to ascertain whether a program is achieving expected benchmarks and outcomes (targets and goals). Frequent measures of quality permit prompt recognition and correction of any unstable component of the screening process (Agency for Healthcare Policy and Research, 1995). Focused reeducation for staff can be undertaken in a timely manner to address strategies to achieve targets and goals.
C. Confirmation of Hearing Loss in Infants Referred From UNHS (Principles 2 and 8)
Infants who meet the defined criteria for referral should receive follow-up audiologic and medical evaluations before 3 months of age. The infant should be referred for comprehensive audiologic assessment and specialty medical evaluations to confirm the presence of hearing loss and to determine type, nature, options for treatment, and (whenever possible) etiology of the hearing loss. After a hearing loss is confirmed, coordination of services should be expedited by the infant's medical home and Individuals with Disabilities Education Act (IDEA) Part C coordinating agencies. Part C agencies are responsible for Child Find and intervention for children with disabilities and the related professionals with expertise in hearing loss evaluation and treatment. The infant's primary care physician, with guidance or coordination from state and local agencies, should address parental concerns and mobilize systems on behalf of the infant and family. Professionals in health care and education must interface to provide families with needed services for the infant with hearing loss.
1. Audiologic Evaluation. Audiologists providing the initial audiologic test battery to confirm the existence of a hearing loss in infants must include physiologic measures and developmentally appropriate behavioral techniques. Adequate confirmation of an infant's hearing status cannot be obtained from a single test measure. Rather, a test battery is required to cross-check results of both behavioral and physiologic measures (Jerger & Hayes, 1976). The purpose of the audiologic test battery is to assess the integrity of the auditory system, to estimate hearing sensitivity, and to identify all intervention options. Regardless of the infant's age, ear-specific estimates of type, degree, and configuration of hearing loss should be obtained.
For infants birth to 6 months of age, the test battery should begin with a child and family history and must include an electrophysiologic measure of threshold such as ABR (Sininger, Abdala, & Cone-Wesson, 1997; Stapells, Gravel, & Martin, 1995) or other appropriate electrophysiologic tests (Rance, Rickards, Cohen, DeVidi, & Clark, 1995) using frequency-specific stimuli. The assessment of the young infant must include OAEs (Prieve, Fitzgerald, Schulte, & Demp, 1997), a measure of middle ear function, acoustic reflex thresholds, observation of the infant's behavioral response to sound, and parental report of emerging communication and auditory behaviors. Appropriate measures of middle ear function for this age group include reflectance (Keefe & Levi, 1996), tympanometry using appropriate frequency probe stimuli (Marchant et al., 1986), bone conduction ABR (Cone-Wesson & Ramirez, 1997), and/or pneumatic otoscopy.
The confirmatory audiologic test battery for infants and toddlers age 6 through 36 months includes a child and family history, behavioral response audiometry (either visual reinforcement or conditioned play audiometry depending on the child's developmental age), OAEs, acoustic immittance measures (including acoustic reflex thresholds), speech detection and recognition measures (Diefendorf & Gravel, 1996; Gravel & Hood, 1999), parental report of auditory and visual behaviors, and a screening of the infant's communication milestones. Physiologic tests, such as ABR, should be performed at least during the initial evaluation to confirm type, degree, and configuration of hearing loss.
In accordance with IDEA, referral to a public agency must take place within 2 working days after the infant has been identified as needing evaluation. Once the public agency receives the referral, its role is to appoint a service coordinator, identify an audiologist to complete the audiologic evaluation, and identify other qualified personnel to determine the child's level of functioning. An IFSP must be held within 45 days of receiving the referral (Public Law 105-17: the amendments to the Individuals with Disabilities Education Act, IDEA 1997; U.S. Department of Education, Office of Special Education and Rehabilitative Services, 1998).
2. Medical Evaluation. Every infant with confirmed hearing loss and/or middle ear dysfunction should be referred for otologic and other medical evaluation. The purpose of these evaluations is to determine the etiology of hearing loss, to identify related physical conditions, and to provide recommendations for medical treatment as well as referral for other services. Essential components of the medical evaluation include clinical history, family history, and physical examination as well as indicated laboratory and radiologic studies. When indicated and with family consent, the otolaryngologist may consult with a geneticist for chromosome analysis and for evaluation of specific syndromes related to hearing loss.
(a) Pediatrician or primary care physician: The infant's pediatrician or other primary care physician is responsible for monitoring the general health and well-being of the infant. In addition, the primary care physician in partnership with the family and other health care professionals, assures that audiologic assessment is conducted on infants who do not pass screening and initiates referrals for medical specialty evaluations necessary to determine the etiology of the hearing loss. Middle-ear status should be monitored because the presence of middle-ear effusion can further compromise hearing. The pediatrician or primary care physician should review the infant's history for presence of risk indicators that require monitoring for delayed onset and/or progressive hearing loss and should insure periodic audiologic evaluation for children at risk. Also, because 30% to 40% of children with confirmed hearing loss will demonstrate developmental delays or other disabilities, the primary care physician should monitor developmental milestones and initiate referrals related to suspected disabilities (Karchmer & Allen, 1999).
(b) Otolaryngologist: The otolaryngologist's evaluation should consist of a comprehensive clinical history; family history; physical assessment, and laboratory tests involving the ears, head, face, neck, and such other systems as skin (pigmentation), eye, heart, kidney, and thyroid that could be affected by childhood hearing loss (Tomaski & Grundfast, 1999). The physical examination of the ear involves identification of external ear malformations including preauricular tags and sinuses, abnormalities or obstruction of ear canals such as the presence of excessive cerumen, and abnormalities of the tympanic membrane and/or middle ear, including otitis media with effusion. Supplementary evaluations may include imaging studies of the temporal bones and electrocardiograms. Laboratory assessments useful for identifying etiology may include urinalysis, blood tests for congenital or early-onset infection (e.g., cytomegalovirus, syphilis, toxoplasmosis), and specimen analyses for genetic conditions associated with hearing loss.
c) Other medical specialists: The etiology of neonatal hearing loss may remain uncertain in as many as 30% to 40% of children. However, most congenital hearing loss is hereditary, and nearly 200 syndromic and nonsyndromic forms have already been identified (Brookhouser, Worthington, & Kelly, 1994). For 20% to 30% of children, there are associated clinical findings that can be of importance in patient management. Where thorough physical and laboratory investigations fail to define the etiology of hearing loss, families should be offered the option of genetic evaluation and counseling by a medical geneticist. The medical geneticist is responsible for the collection and interpretation of family history data, the clinical evaluation and diagnosis of inherited diseases, the performance and assessment of genetic tests, and the provision of genetic counseling. Geneticists are qualified to interpret the significance and limitations of new tests and to convey the current status of knowledge during genetic counseling.
Other medical specialty areas, including developmental pediatrics, neurology, ophthalmology, cardiology and nephrology, may be consulted to determine the presence of related body-system disorders as part of syndromes associated with hearing loss. In addition, every infant with hearing loss should receive an ophthalmologic evaluation at regular intervals to rule out concomitant late-onset vision disorders (Gallaudet University Center for Assessment and Demographic Study, 1998; Johnson, 1999). Many infants with hearing loss will have received care in an NICU. Because NICU-enrolled infants will demonstrate other developmental disorders, the assistance of a developmental pediatrician may be valuable for management of these infants.
3. Benchmarks and quality indicators for the confirmation of hearing loss.
(a) Benchmarks
There are few published data available to provide targets for programs involved in confirmation of hearing loss. Until benchmark data that provide a goal are published, programs should strive to provide care to 100% of infants needing services.
1. Comprehensive services for infants and families referred following screening are coordinated between the infant's medical home, family, and related professionals with expertise in hearing loss and the state and local agencies responsible for provision of services to children with hearing loss.
2. Infants referred from UNHS begin audiologic and medical evaluations before 3 months of age or 3 months after discharge for NICU infants (Dalzell et al., 2000).
3. Infants with evidence of hearing loss on audiologic assessment receive an otologic evaluation.
4. Families and professionals perceive the medical and audiologic evaluation process as positive and supportive.
5. Families receive referral to Part C coordinating agencies, appropriate intervention programs, parent/consumer and professional organizations, and child-find coordinators if necessary.
(b) Associated quality indicators of the confirmation of hearing loss component of the EHDI programs may include the following:
1. Percentage of infants and families whose care is coordinated between the medical home and related professionals.
2. Percentage of infants whose audiologic and medical evaluations are obtained before an infant is 3 months of age.
3. Percentage of infants with confirmed hearing loss referred for otologic evaluation.
4. Percentage of families who accept audiologic and medical evaluation services.
5. Percentage of families of infants with confirmed hearing loss that have a signed IFSP by the time the infant reaches 6 months of age.
D. Early Intervention (Principles 3 and 8)
The mounting evidence for the crucial nature of early experience in brain development provides the impetus to ensure learning opportunities for all infants (Kuhl et al., 1997; Kuhl, Williams, Lacerda, Stevens, & Lindblom, 1992; Sininger, Doyle, & Moore, 1999). Research demonstrates that intensive early intervention can alter positively the cognitive and developmental outcomes of young infants with disabilities or infants who are socially and economically disadvantaged (Guralnick, 1997; Infant Health and Development Program, 1990; Ramey & Ramey, 1992, 1998). Yoshinaga-Itano, Sedey, Coulter, and Mehl (1998), Moeller (in press), and Carney and Moeller (1998) have corroborated these findings in infants with hearing loss.
1. Early Intervention Program Development. Early intervention services should be designed to meet the individualized needs of the infant and family, including addressing acquisition of communicative competence, social skills, emotional well-being, and positive self-esteem (Karchmer & Allen, 1999). Six frequently cited principles of effective early intervention are (1) developmental timing, (2) program intensity, (3) direct learning, (4) program breadth and flexibility, (5) recognition of individual differences, and (6) environmental support and family involvement (Meadow-Orleans, Mertens, Sass-Lehrer, & Scott-Olson, 1997; Moeller & Condon, 1994; Ramey & Ramey, 1992, 1998; Stredler-Brown, 1998; Thomblin, Spencer, Flock, Tyler, & Gantz, 1999).
Developmental timing refers to the age at which services begin and the duration of enrollment. Programs that enroll infants at younger ages and continue longer are found to produce the greatest benefits. Program intensity refers to the amount of intervention and is measured by multiple factors, such as the number of home visits/contacts per week for the infant and the family's participation in intervention. Greater developmental progress occurs when the infant and family are actively and regularly involved in the intervention. The principle of direct learning encompasses the idea that center-based and home-based learning experiences are more effective when there is direct (provided by trained professionals) as well as indirect intervention. The principle of program breadth and flexibility notes that successful intervention programs offer a broad spectrum of services and are flexible and multifaceted to meet the unique needs of the infant and family. Rates of progress and benefits from programs are functions of infant and family individual differences; not everyone progresses at the same rate nor benefits from programs to the same extent. Finally, the benefits of early intervention continue over time depending on the effectiveness of existing supports: family involvement and other environmental supports (e.g., home, school, health, and peer) (Ramey & Ramey, 1992). Individualization in intervention tailors the services to be developmentally appropriate and recognizes meaningful individual and family differences (Cohen, 1993, 1997).
Optimal intervention strategies for the infant with any hearing loss require that intervention begin as soon as there is confirmation of a permanent hearing loss to enhance the child's acquisition of developmentally appropriate language skills. All infants with the targeted hearing loss are at risk for delayed communication development and should receive early intervention services (Bess, Dodd-Murphy, & Parker, 1998; Rushmer, 1992). Early intervention provides appropriate services for the child with hearing loss and assures that families receive consumer-oriented information. Documented discussion must occur about the full range of resources in early intervention and education programs for children with hearing loss.
In supplying information to families, professionals must recognize and respect the family's natural transitions through the grieving process at the time of initial diagnosis of hearing loss and at different intervention decision-making stages (Cherow, Dickman, & Epstein, 1999; Luterman, 1985; Luterman & Kurtzer-White, 1999). The range of intervention options should be reviewed at least every 6 months. Families should be apprised of individuals who and organizations that can enhance informed decision-making such as peer models, persons who are hard of hearing and deaf, and consumer and professional associations (Baker-Hawkins & Easterbrooks, 1994; Cherow, Dickman, & Epstein, 1999).
Early intervention must be preceded by a comprehensive assessment of the infant's and family's needs and the family's informed decision-making related to those needs (Stredler-Brown & Yoshinaga-Itano, 1994). Federal law provides funds for states to participate in early intervention services for infants with hearing loss (Public Law 105-17: the amendments to the Individuals with Disabilities Education Act, IDEA 1997; U.S. Department of Education, Office of Special Education and Rehabilitative Services, 1998). Part C of IDEA requires that an interdisciplinary developmental evaluation be completed to determine the child's level of functioning in each of the following developmental areas: cognitive, physical, and communicative development; social or emotional development; and adaptive development (34 C.F.R. Part 303 §303.322). The IFSP is to be developed by the family and service coordinator (Joint Committee of ASHA and Council on Education of the Deaf, 1994). The IFSP specifies needs, outcomes, intervention components, and anticipated developmental progress. The full evaluation process must be completed within 45 days of primary referral. However, intervention services may commence before completion of the full evaluation of all developmental areas and during the confirmation of the hearing loss if parent/guardian consent is obtained and an interim IFSP is developed (Matkin, 1988). Once services are begun, ongoing assessment of progress is crucial to determine appropriateness of the intervention strategies. In addition, the family and service coordinator must review the IFSP at least every 6 months to determine whether progress toward achieving the outcomes is being made and whether the outcomes should be modified or revised. The IFSP must be evaluated at least annually and–taking into consideration the results of any current evaluations, progress made, and other new information, revised as appropriate (34 CFR Part 303 §303.342).
Thirty to 40% of children with hearing loss demonstrate additional disabilities that may have concomitant effects on communication and related development (Gallaudet University Center for Assessment and Demographic Study, 1998; Schildroth & Hotto, 1993). Thus, interdisciplinary assessment and intervention are essential to address the developmental needs of all children who are hard of hearing or deaf, especially those with additional developmental disabilities (Cherow, Dickman, & Epstein, 1999; Cherow, Matkin, & Trybus, 1985).
The diverse demographics of infants with hearing loss and their families highlight the importance of shaping the early intervention curriculum to the infant and family profile (Calderon, Bargones, & Sidman, 1998; Karchmer & Allen, 1999). Families who live in underserved areas may have less accessibility, fewer professional resources, deaf or hard of hearing role models, or sign language interpreters available to assist them. A growing number of children with hearing loss in the United States are from families that are non-native English speaking (Baker-Hawkins & Easterbrooks, 1994; Christensen & Delgado, 1993; Cohen, 1997; Cohen, Fischgrund, & Redding, 1990; Scott, 1998). These factors underscore the necessity of providing comprehensive, culturally sensitive information to families–information that is responsive to their needs and that results in informed choices (Schwartz, 1996).
2. Audiologic Habilitation. The vast majority of infants and children with bilateral hearing loss benefit from some form of personal amplification or sensory device (Pediatric Working Group of the Conference on Amplification for Children with Auditory Deficits, 1996). If the family chooses individualized personal amplification for their infant, hearing aid selection and fitting should be provided by the audiologist in a timely fashion. Delay between confirmation of the hearing loss and amplification should be minimized (Arehart, Yoshinaga-Itano, Thomson, Gabbard, & Stredler Brown, 1998).
Hearing aid fitting proceeds optimally when the results of the medical evaluation and physiologic (OAE and ABR) and behavioral audiologic assessments are in accord. However, the provision of amplification should proceed based on physiologic measures alone if behavioral measures of threshold are precluded because of the infant's age or developmental level. In such cases, behavioral measures should be obtained as soon as possible to corroborate the physiologic findings. The goal of amplification fitting is to provide the infant with maximum access to the acoustic features of speech within a listening range that is safe and comfortable. That is, amplified speech should be comfortably above the infant's sensory threshold, but below the level of discomfort across the speech frequency range for both ears (Pediatric Working Group of the Conference on Amplification for Children with Auditory Deficits, 1996).
The amplification fitting protocol should combine prescriptive procedures that incorporate individual real-ear measurements (Pediatric Working Group of the Conference on Amplification for Children with Auditory Deficits, 1996). These techniques allow amplification to be individually fitted to meet the unique characteristics of each infant's hearing loss. Validation of the benefits of amplification, particularly for speech perception, should be examined in the infant's typical listening environments. Complementary or alternative sensory technology (FM systems, vibrotactile aids, or cochlear implants) may be recommended as the primary and/or secondary listening device, depending on the degree of the infant's hearing loss, goals of auditory habilitation, acoustic environments, and family's informed choices (ASHA, 1991). Long-term monitoring of personal amplification requires audiologic assessment; electroacoustic, real-ear, and functional checks of the amplification/listening device, as well as refinement of the prescriptive targets. Long-term monitoring also includes continual validation of communication, social-emotional, cognitive, and later academic development to assure that progress is commensurate with the infant's abilities. The latter data are obtained through interdisciplinary evaluation and collaboration by the IFSP team that includes the family.
The impact of otitis media with effusion (OME) is greater for infants with sensorineural hearing loss than those with normal cochlear function. Sensory or permanent conductive hearing loss is compounded by additional conductive hearing loss associated with OME. OME further reduces access to auditory/oral language stimulation and spoken language development for infants whose families choose an auditory-oral approach to communication development. Prompt referral to otolaryngologists for treatment of persistent or recurrent OME is indicated in infants with sensorineural hearing loss. Ongoing medical/surgical management of OME may be needed to resolve the condition. Management of OME, however, should not delay the prompt fitting of amplification unless there are medical contraindications (Brookhouser, Worthington, & Kelly, 1994).
3. Medical and Surgical Intervention. Medical intervention is the process by which a physician provides medical diagnosis and direction for medical and/or surgical treatment options for hearing loss and/or related medical disorder(s) associated with hearing loss. Treatment varies from the removal of cerumen and the treatment of otitis media with effusion to long-term plans for reconstructive surgery and assessment of candidacy for cochlear implants. If necessary, surgical treatment of malformation of the outer and middle ears should be considered in the intervention plan for infants with conductive or sensorineural plus conductive hearing loss. Cochlear implants may be an option for certain children age 12 months and older with profound hearing loss who show limited benefit from conventional amplifications. As noted above, in infants with identified sensorineural hearing loss, the presence of otitis media needs to be recognized promptly and treated, with the infant monitored on a periodic basis.
4. Communication Assessment and Intervention. Language is acquired with greater ease during certain sensitive periods of infants' and toddlers' development (Clark, 1994; Mahshie, 1995). The process of language acquisition includes learning the precursors of language, such as the rules pertaining to selective attention and turn taking (Kuhl et al., 1997; Kuhl, Williams, Lacerda, Stevens, & Lindblom, 1992). Cognitive, social, and emotional developments depend on the acquisition of language. Development in these areas is synergistic. A complete language evaluation should be performed for infants and toddlers with hearing loss. The evaluation should include an assessment of oral, manual, and/or visual mechanisms as well as cognitive abilities.
A primary focus of early intervention programs is to support families in developing the communication abilities of their infants and toddlers who are hard of hearing or deaf (Carney & Moeller, 1998). Elements of oral and sign language development include vocal/manual babbling, vocal/visual turn-taking, and early word/sign acquisition. Oral and/or sign language development should be commensurate with the child's age and cognitive abilities and should include acquisition of phonologic (for spoken language), visual/spatial/motor (for signed language), morphologic, semantic, syntactic, and pragmatic skills.
Early interventionists should follow family-centered principles to assist in developing communicative competence of infants and toddlers who are hard of hearing or deaf (Baker-Hawkins and Easterbrooks, 1994; Bamford, 1998; Fisher, 1994). Families should be provided with information specific to language development and with family-involved activities that facilitate language development. Early interventionists should ensure access to peer and language models. Peer models might include families with normal hearing children as well as children or adults who are hard of hearing and deaf as appropriate to the needs of the infant with hearing loss (Marschark, 1997; Thompson, 1994). Depending on informed family choices, peer models could include users of visual language (e.g., American Sign Language) and other signed systems as well as users of auditory/oral communication methods for spoken language development (Pollack, Goldberg, & Coleffe-Schenck, 1997). Information on visual communication methods such as American Sign Language, other signed systems, and cued speech should be provided. Information on oral/auditory language, personal hearing aids, and assistive devices such as FM systems, tactile aids, and cochlear implants should also be made available.
The specific goals of early intervention are to facilitate developmentally appropriate language skills, enhance the family's understanding of its infant's strengths and needs, and promote the family's ability to advocate for its infant. Early intervention should also build family support and confidence in parenting the infant who is deaf or hard of hearing and increase the family's satisfaction with the EHDI process (Fisher, 1994; U.S. Department of Education, Office of Special Education and Rehabilitative Services, 1998). Provision of early intervention services includes monitoring participation and progress of the infant and family as well as adapting and modifying interventions as needed. Systematic documentation of the intervention approach facilitates decision-making on program changes.
5. Benchmarks and Quality Indicators for Early Intervention Programs.
(a) Benchmarks
It should be the goal of the intervention component of an EHDI program that all infants be served as described below. Because specific benchmarks for early intervention have yet to be reported, target percentages are not noted here. The JCIH strongly recommends that these data be obtained so that benchmarks may be made available.
- Infants with hearing loss are enrolled in a family-centered early intervention program before 6 months of age.
- Infants with hearing loss are enrolled in a family-centered early intervention program with professional personnel who are knowledgeable about the communication needs of infants with hearing loss.
- Infants with hearing loss and no medical contraindication begin use of amplification when appropriate and agreed on by the family within 1 month of confirmation of the hearing loss.
- Infants with amplification receive ongoing audiologic monitoring at intervals not to exceed 3 months.
- Infants enrolled in early intervention achieve language development in the family's chosen communication mode that is commensurate with the infant's developmental level as documented in the IFSP and that is similar to that for hearing peers of a comparable developmental age.
- Families participate in and express satisfaction with self-advocacy.
(b) Quality indicators for the intervention services may include the following:
- Percentage of infants with hearing loss who are enrolled in a family-centered early intervention program before 6 months of age
- Percentage of infants with hearing loss who are enrolled in an early intervention program with professional personnel who are knowledgeable about overall child development as well as the communication needs and intervention options for infants with hearing loss
- Percentage of infants in early intervention who receive language evaluations at 6-month intervals
- Percentage of infants and toddlers whose language levels, whether spoken or signed, are commensurate with those of their hearing peers
- Percentage of infants and families who achieve the outcomes identified on their IFSP
- Percentage of infants with hearing loss and no medical contraindication who begin use of amplification when agreed on by the family within 1 month of confirmation of the hearing loss
- Percentage of infants with amplification who receive ongoing audiologic monitoring at intervals not to exceed 3 months.
- Number of follow-up visits for amplification monitoring and adjustment within the first year following amplification fitting
- Percentage of families who refuse early intervention services
- Percentage of families who participate in and express satisfaction with self-advocacy
E. Continued Surveillance of Infants and Toddlers (Principle 4)
Since 1972, the JCIH has identified specific risk indicators that often are associated with infant and childhood hearing loss. These risk indicators have been applied both in the United States and in other countries and serve two purposes. First, risk indicators help identify infants who should receive audiologic evaluation and who live in geographic locations (e.g., developing nations, remote areas) where universal hearing screening is not yet available. The JCIH no longer recommends programs calling for screening at-risk infants because such programs will identify approximately 50% of infants with hearing loss; however, these programs may be useful where resources limit the development of universal newborn hearing screening. Second, because normal hearing at birth does not preclude delayed onset or acquired hearing loss, risk indicators help identify infants who should receive on-going audiologic and medical monitoring and surveillance.
Risk indicators can be divided into two categories: those present during the neonatal period and those that may develop as a result of certain medical conditions or essential medical interventions in the treatment of an ill child. Risk indicators published in the 1994 Position Statement are revised in 2000 to take account of current information. Specifically, data have been considered from an epidemiological study of permanent childhood hearing impairment in the Trent Region of Great Britain from 1985 through 1993 (Fortnum & Davis, 1997) and the recent NIH multicenter study, "Identification of Neonatal Hearing Impairment" (Norton et al., in press). Cone-Wesson et al. (in press) analyzed the prevalence of risk indicators for infants identified with hearing loss in that study. Three thousand one hundred thirty-four infants evaluated during their initial birth hospitalization were reevaluated for the presence of hearing loss between 8 and 12 months of age. The majority of these infants were NICU graduates (2,847), and the remaining 287 infants had risk indicators for hearing loss that did not require intensive care, such as family history or craniofacial anomalies. Infants with history or evidence of transient middle ear dysfunction were excluded from the final analysis, revealing 56 with permanent hearing loss.
Cone-Wesson et al. (in press) determined the prevalence of hearing loss for each risk factor by dividing the number of infants with the risk factor and hearing loss by the total number of infants in the sample with a given risk factor. Hearing loss was present in 11.7% of infants with syndromes associated with hearing loss, which included Trisomy 21; Pierre Robin syndrome; CHARGE syndrome; choanal atresia; Rubinstein-Taybi syndrome; Stickler syndrome; and oculo-auriculo-vertebral (OAV) spectrum (also known as Goldenhar syndrome). Family history of hearing loss had a prevalence of 6.6%, meningitis 5.5%, and craniofacial anomalies 4.7%. In contrast, infants treated with aminogycoside antibiotics had a prevalence of hearing loss of only 1.5%, consistent with data of Finitzo-Hieber, McCracken, & Brown (1985). Analyzing risk indicators, such as ototoxicity, by prevalence points out that although a large number of NICU infants with hearing loss have a history of aminogycoside treatment, only a small percentage of those receiving potentially ototoxic antibiotics actually incurred hearing loss. In fact, 45% of infants treated in the NICU received such treatment (Vohr et al., in press).
1. Given these current data, the JCIH risk indicators have been modified for use in neonates (birth through age 28 days) where universal hearing screening is not yet available. These indicators are as follows:
(a) An illness or condition requiring admission of 48 hours or greater to a NICU (Cone-Wesson et al., in press; Fortnum & Davis, 1997).
(b) Stigmata or other findings associated with a syndrome known to include a sensorineural and or conductive hearing loss (Cone-Wesson et al., in press).
(c) Family history of permanent childhood sensorineural hearing loss (Cone-Wesson et al., in press; Fortnum & Davis, 1997).
(d) Craniofacial anomalies, including those with morphological abnormalities of the pinna and ear canal (Cone-Wesson et al., in press; Fortnum & Davis, 1997).
(e) In utero infection such as cytomegalovirus, herpes, toxoplasmosis, or rubella (Demmler, 1991; Littman, Demmler, Williams, Istas, & Griesser, 1995; Williamson, Demmler, Percy, & Catlin, 1992).
Interpretation of the Cone-Wesson et al. (in press) data reveals that 1 of 56 infants identified with permanent hearing loss revealed clear evidence of late-onset hearing loss by 1 year of age. The definition of late-onset hearing loss for this analysis was a present ABR at 30 dB in the newborn period and hearing thresholds by visual reinforcement audiometry at age 8-12 months >40 dB for all stimuli. The infant with late-onset loss passed screening ABR, TOAE, and DPOAE during the newborn period but had reliable behavioral thresholds revealing a severe hearing loss at 1 year of age. Risk indicators for this infant included low birthweight, respiratory distress syndrome, bronchio-pulmonary dysplasia, and 36 days of mechanical ventilation. Although these data are valuable, additional study of large samples of infants is needed before risk indicators for progressive or delayed-onset hearing loss can be clearly defined.
2. The JCIH recommends the following indicators for use with neonates or infants (29 days through 2 years). These indicators place an infant at risk for progressive or delayed-onset sensorineural hearing loss and/or conductive hearing loss. Any infant with these risk indicators for progressive or delayed-onset hearing loss who has passed the birth screen should, nonetheless, receive audiologic monitoring every 6 months until age 3 years. These indicators are as follows:
(a) Parental or caregiver concern regarding hearing, speech, language, and or developmental delay.
(b) Family history of permanent childhood hearing loss (Grundfast, 1996).
(c) Stigmata or other findings associated with a syndrome known to include a sensorineural or conductive hearing loss or eustachian tube dysfunction.
(d) Postnatal infections associated with sensorineural hearing loss including bacterial meningitis (Ozdamar, Kraus, & Stein, 1983).
(e) In utero infections such as cytomegalovirus, herpes, rubella, syphilis, and toxoplasmosis.
(f) Neonatal indicators–specifically hyperbilirubinemia at a serum level requiring exchange transfusion, persistent pulmonary hypertension of the newborn associated with mechanical ventilation, and conditions requiring the use of extracorporeal membrane oxygenation (ECMO) (Roizen, 1999).
(g) Syndromes associated with progressive hearing loss such as neurofibromatosis, osteopetrosis, and Usher's syndrome.
(h) Neurodegenerative disorders, such as Hunter syndrome, or sensory motor neuropathies, such as Friedreich's ataxia and Charcot-Marie-Tooth syndrome.
(i) Head trauma.
(j) Recurrent or persistent otitis media with effusion for at least 3 months (Stool et al. 1994).
Because some important indicators, such as family history of hearing loss, may not be determined during the course of UNHS programs, the presence of all late-onset risk indicators should be determined in the medical home during early well-baby visits. Those infants with significant late-onset risk factors should be carefully monitored for normal communication developmental milestones during routine medical care.
The JCIH recommends ongoing audiologic and medical monitoring of infants with unilateral, mild, or chronic conductive hearing loss. Infants and children with mild or unilateral hearing loss may also experience adverse speech, language, and communication skill development, as well as difficulties with social, emotional, and educational development (Bess, Dodd-Murphy, & Parker, 1998; Blair, Petterson, & Viehweg, 1985; Davis, Elfenbein, Schum, & Bentler, 1986; Matkin & Bess, 1998; Roush & Matkin, 1994; Tharpe & Bess, 1995). Infants with unilateral hearing loss are at risk for progressive and/or bilateral hearing loss (Brookhouser, Worthington, & Kelly, 1994). Infants with frequent episodes of OME also require additional vigilance to address the potential adverse effects of fluctuating conductive hearing loss associated with persistent or recurrent OME (Friel-Patti & Finitzo, 1990; Friel-Patti, Finitzo, Meyerhoff, & Hieber, 1986; Friel-Patti, Finitzo-Hieber, Conti, & Brown, 1982; Gravel & Wallace, 1992; Jerger, Jerger, Alford, & Abrams, 1983; Roberts, Burchinal, & Medley, 1995; Stool et al., 1994; Wallace et al., 1988).
The population of infants cared for in the NICU may also be at increased risk for neural conduction and/or auditory brainstem dysfunction, including auditory neuropathy. Auditory neuropathy is a recently identified disorder, characterized by a unique constellation of behavioral and physiologic auditory test results (Gravel & Stapells, 1993; Kraus, Ozdamar, Stein, & Reed, 1984; Sininger, Hood, Starr, Berlin, & and Picton, 1995; Starr, Picton, Sininger, Hood, & Berlin, 1996; Stein et al., 1996). Behaviorally, children with auditory neuropathy have been reported to exhibit mild-to-profound hearing loss and poor speech perception. Physiologic measures of auditory function (e.g., otoacoustic emissions and auditory brainstem response) demonstrate the finding of normal OAEs (suggesting normal outer hair cell function) and atypical or absent ABRs (suggesting neural conduction dysfunction). Reports suggest that those at increased risk for auditory neuropathy are (a) infants with a compromised neonatal course who receive intensive neonatal care (Berlin et al., 1999; Stein et al., 1996), (b) children with a family history of childhood hearing loss (Corley & Crabbe, 1999), and (c) infants with hyperbilirubinemia (Stein et al., 1996). Currently, neither the prevalence of auditory neuropathy in newborns nor the natural history of the disorder is known, and treatment options are not well defined. Audiologic and medical monitoring of infants at risk for auditory neuropathy is recommended. Infants with these disorders can be detected only by the use of OAE and ABR technology used in combination. Prospective investigations of this neural conduction disorder are warranted (see Future Directions).
F. Protection of Infants' and Families' Rights (Principles 5 and 6)
Each agency or institution involved in the EHDI process shares the responsibility for protecting infant and family rights. These rights include access to UNHS, information in the family's native language, choice, and confidentiality (NIDCD, 1999). Families should receive information about childhood hearing loss in consumer-oriented language. The information should cover the prevalence and effects of early hearing loss, the potential benefits and risks of screening and evaluation procedures, and the prognosis with and without early identification and intervention. Alternative funding sources should be sought if the parent(s) or legal guardian desires to have the infant screened for hearing loss but does not have a reimbursement option.
Families have the same right to accept or decline hearing screening or any follow-up care for their newborn as they do any other screening or evaluation procedures or intervention. Implied or written consent consistent with the protocol of the hospital or the requirements of the state should be obtained for newborn hearing screening after determining the family or legal guardian have been provided appropriate educational materials and have had their questions answered by qualified health care personnel.
The results of screening are to be communicated verbally and in writing to families by health care professionals knowledgeable about hearing loss and the appropriate interpretation of the screening results. EHDI data merit the same level of confidentiality and security afforded all other health care and education information in practice and law. The newborn and his or her family have the right to confidentiality of the screening and follow-up assessments and the acceptance or rejection of suggested intervention(s). Consent of the parent or guardian is the basic legal requisite for disclosure of medical information. In compliance with federal and state laws, mechanisms should be established that assure parental release and approval of all communications regarding the infant's test results, including those to the infant's medical home and early intervention coordinating agency and programs. Confidentiality requires that family and infant information not be transmitted or accessible in unsecured data formats. An effective information system is a tool to assure both proper communication and confidentiality of EHDI information.
G. Information Infrastructure (Principles 7 and 8)
In concert with the 1994 Position Statement (JCIH, 1994a,b), the JCIH recommends development of uniform state registries and national information databases incorporating standardized methodology, reporting, and system evaluation. The choice of an information management system affects what questions can be answered and what tools are available for infant and family management and for program evaluation and reporting (Pool, 1996). Management and use of information generated by newborn hearing screening, evaluation, and intervention programs require careful consideration by service providers, state-specific lead coordinating agencies, statewide advisory committees, and state and federal funding and regulatory agencies. Federal and state agencies need to standardize data definitions to ensure the value of state registries and federal data sets and to prevent misleading or unreliable information (O'Neal, 1997). Information management should be used to improve services to infants and their families; to assess the quality of screening, evaluation, and intervention; and to facilitate collection of data on demographics of neonatal and infant hearing loss.
To achieve the first goal of improving services to infants and their families, multiple system components (e.g., hospitals, practitioners, public health, and public and private education agencies) that provide care for infants and families should be integrated. Optimally, and within the limits of confidentiality as defined by state regulation and parental informed consent, each service provider within the EHDI system (e.g., hospital, practitioner, public health agency, and public and private education agencies) participates in information management in order to track elements of care to each infant and family. The information obtained while using an effective information management system allows for the accurate and timely description of services provided to each infant and documents recommendations for follow-up and referral to other providers. Such information permits prospective monitoring of outcomes for each infant screened and assures that each infant is connected to the services he or she needs.
In addition to ensuring that each infant receives all needed services, effective information management is used to promote program measurement and accountability. Although recent survey data suggest that hospitals are successfully initiating universal screening, EHDI services including confirmation of hearing loss, fitting of amplification, and initiation of early intervention remain delayed (Arehart, Yoshinaga-Itano, Thomson, Gabbard, & Stredler Brown, 1998). One factor contributing to the delay beyond the 1994 and 2000 JCIH recommendations may be that few states have mandatory statewide information management, similar to that described here, that is capable of spanning the entire EHDI process (Hayes, 1999).
The information obtained from the information management system should assist both the individual provider and the lead coordinating agency in measuring quality indicators associated with program services (e.g., screening, evaluation, and/or intervention). Those professionals closest to the process should be responsible for program evaluation using the benchmarks and quality indicators suggested in this document. The information system should provide the measurement tools to determine the degree to which each process (e.g., screening, evaluation, and intervention) is stable, sustainable, and conforms to program benchmarks. Timely and accurate monitoring of relevant quality measures is essential.
Effective information management is capable of aggregating individual infant data from multiple EHDI service providers including hospitals, practitioners, public health agencies, and public and private education agencies. This information provides the basis for evaluating the effectiveness of the EHDI programs in meeting program goals of universal screening, prompt evaluation, and early and effective intervention. Tracking families through the systems of screening, evaluation, and intervention will permit quantification of the number of infants requiring and receiving services, and document the types of service during a specific period. Tracking improves the ability to identify infants who are lost to follow-up at any stage of the EHDI process. Until centralized statewide tracking, reporting, and coordination are mandatory, the transition of infants and families from screening to confirmation of hearing loss to intervention will continue to be problematic (Diefendorf & Finitzo, 1997).
The JCIH endorses the concept of a national database to permit documentation of the demographics of neonatal hearing loss, including prevalence and etiology across the United States. The development of a national database, in which aggregate state data reside, is achievable only with standardization of data elements and definitions (O'Neal, 1997). Standardized data management systems will ensure that appropriate data are collected and transmitted from statewide EHDI programs to the national data system. Data transmitted from the states to the federal level need not include individually identifiable patient or family information.
The request for information moves from the federal level to the state level and from the state to the hospitals and practitioners. Requirements from federal levels drive what data are collected and maintained at the state and hospital level. The flow of information should move from the hospital and practitioner to the state and federal levels through an integrated information system. Hospitals may collect and monitor data not required at the state level. Not all data collected as part of a universal newborn hearing screening program at the hospital or by the practitioner are needed at the state level, especially for the infant who passes the birth hearing screening with no risk indicators. Similarly, states may choose to collect data and monitor an expanded data set not required at the federal level. Information on the care status of an individual infant is not needed at the federal level.
The Bureau of Maternal and Child Health (MCHB) currently requires that each state report two data items: the number of live births and the number of newborns screened for hearing loss during the birth admission. The Centers for Disease Control and Prevention (CDC) are requesting that states submit 10 data items. CDC in conjunction with the Directors of Speech and Hearing Programs in State Health and Welfare Agencies (DSHPSHWA)began a pilot effort in 1999 to assess the feasibility and logistics of developing and reporting a national EHDI data set. The Pilot National Data Set includes the number of birthing hospitals in the state and the number of hospitals with universal hearing screening programs; the number of live births in the state and the number of infants screened for hearing loss before discharge from the hospital; the number of infants referred for audiologic evaluation before 1 month of age and the number with an audiologic evaluation before 3 months; the number of infants with permanent congenital hearing loss; the mean, median, and minimum age of diagnosis of hearing loss for infants identified in a newborn hearing screening program; and the number of infants with permanent hearing loss receiving intervention by 6 months. Such data could be used to examine prevalence of hearing loss by state or region, to support legislation for services to infants who are hard of hearing and deaf and their families, and to provide national benchmarks and quality indicators.
IV. Future Directions
New opportunities and challenges are presented by the current efforts directed at the early identification, assessment, and intervention for newborns and very young infants with hearing loss. Ultimately, the development of communication skills commensurate with cognitive abilities and cultural beliefs in the preferred modality of the family is the goal for all infants and children who are hard of hearing and deaf. Achievement of this goal will permit these children to avail themselves of all educational, social, and vocational opportunities in order to achieve full participation in society across the life span. To assure that such opportunities are available, universities should assume responsibility for special-track, interdisciplinary, professional education programs on early intervention for the child who is deaf or hard of hearing. Universities should also introduce training in family systems, the grieving process, cultural diversity, and Deaf culture.
Early identification efforts will be enhanced by the new technology designed specifically for the detection of hearing loss in the newborn period. The growing demand for screening programs will necessitate screening technology that is both rapid and highly reliable. Techniques or combinations of techniques will be required to identify the site of the hearing loss (conductive, cochlear, or neural). The development of middle ear reflectance measures may someday enable screening programs to determine accurately if middle ear dysfunction is contributing to the screening test outcome.
Because of newborn hearing screening, it will be possible to determine what proportion of early onset hearing losses are truly congenital versus those that occur postnatally. It will be possible to determine which types of hearing losses are stable as opposed to fluctuating and/or progressive. Intervention strategies could be tailored to the expected clinical course for each infant. Intervention will also be aimed at preventing the onset or delaying the progression of sensorineural hearing losses. Thus, objective techniques must be developed to assess the integrity and physiology of the inner ear.
Increasing reports of the deleterious effects of auditory neuropathy support the need for prospective studies in large birth populations to determine its prevalence and natural history (Gravel & Stapells, 1993; Kraus, Ozdamar, Stein, & Reed, 1984; Sininger, Hood, Starr, Berlin, & and Picton, 1995; Starr, Picton, Sininger, Hood, & Berlin, 1996; Stein et al., 1996). Consensus development is needed concerning appropriate early intervention strategies for infants with auditory neuropathy. As more information on this disorder becomes available, hearing screening protocols may need to be revised in order to allow the detection of auditory neuropathy in newborns.
The JCIH anticipates that the earliest audiologic assessments, and subsequently the determination of appropriate interventions, will continue to rely on the use of physiologic measures. In particular, ABR air- and bone-conduction techniques could be used for rapid, reliable, and frequency-specific threshold assessment. The further development of these techniques for use with very young infants would be useful in the early comprehensive assessment process. Timely evaluation of hearing sensitivity will prevent delay in confirming the existence of a hearing loss and initiating appropriate audiologic, medical/surgical, and developmental intervention.
Amplification fitting will rely on pediatric prescriptive formulas individualized with real-ear measures and modifications (such as real-ear-to-coupler differences) to select and evaluate hearing aid fittings. Technological advances in digital and programmable hearing aids and alternative strategies such as frequency transposition hearing aids will facilitate more effective early intervention. The age of cochlear implantation for profoundly deaf children may be lowered proportionately with the earlier age of identification. Accurate selection and fitting of these devices in the infant or very young child will require reliance on objective (physiologic) assessment tools as well. These predictive measures, such as electrical ABR or electrical middle ear muscle reflexes obtained with stimulation delivered via the implant, must be validated in older children and adults to prepare for use in infants and prelinguistic children.
Health, social service, and education agencies associated with early intervention and Head Start programs should be prepared for a dramatic escalation in the need for family-centered infant intervention services. Because of the early identification and intervention programs, the JCIH anticipates that children who are hard of hearing and deaf who have received early identification and intervention will perform quite differently from their later-identified peers. As these children enter formal education, systems will need the flexibility to assess and respond to the abilities of these children appropriately.
With advances in human genetic research and the completion of the national Human Genome Project, thousands of genes associated with a variety of conditions will be discovered in the coming decade (Khoury, 1999). The identification of 11 genes for nonsyndromic deafness reported by the end of 1998 (Morton, 1999) provides the impetus for formulating strategies for population-based studies in the genetics of hearing loss. Although many different genes may be associated with nonsyndromic deafness, research indicates that a few of these genes may be responsible for a significant percentage of these cases. DFNB1, which is a gene responsible for recessive, nonsyndromic, sensorineural hearing loss, has been found to cause approximately 15% of all infant hearing loss (Cohn et al., 1999; Denoyelle, 1999). Currently, tests for the common mutations will detect 95% of DFNB1 in Caucasian families without consanguinity (Green et al., 1999). A positive test outcome for DFNB1 will eliminate the need for a CT scan, perchlorate washout, and tests for retinitis pigmentosa.
Studies in the genetics of hearing loss could facilitate diagnosis, including identification of risk indicators for progressive or delayed-onset hearing loss. Advanced knowledge regarding recessive genes responsible for nonsyndromic hearing loss could dramatically reduce the number of children whose hearing loss is classified as etiologically unknown. Increased sophistication in diagnosis may lead to new techniques for medical and/or surgical intervention. Otobiological research into hair cell regeneration and protection may yield intervention strategies that can be employed to protect the sensory mechanisms from damage by environmental factors, such as chemotherapeutic agents or high levels of noise or progressive forms of hearing loss.
The public health issues, as well as the ethical and policy implications, involved in this type of research must be addressed. The perspectives of individuals who are hard of hearing and deaf must play a significant role in developing policies regarding the appropriate use of genetic testing and counseling for families who carry genes associated with hearing loss (Brick, 1999). Privacy issues, including the potential impact of this knowledge on educational and vocational opportunities, together with insurability, must be thoroughly considered.
These efforts will be facilitated by the federal government's new goals in Healthy People 2010, which are as follows:
- To increase to 100 the proportion of newborns served by state-sponsored early hearing detection and intervention programs.
- To provide 100 of newborns access to screening.
- To provide follow-up audiologic and medical evaluations before 3 months for infants requiring care.
- To provide access to intervention before 6 months for infants who are hard of hearing and deaf.
We must assure quality in EHDI services through available benchmarks and standards for each stage of the EHDI process. Accountability for the outcomes of audiologic and medical evaluation and intervention services as well as the screening process itself must be documented. Outcomes and quality indicators obtained at the hospital, community, state, and national levels should permit the community to draw conclusions about the EHDI process, including its fiscal accountability (Carpenter, Bender, Nash, & Cornman, 1996). Such information requires that data collection be standardized, prospective, and ongoing for the next decades. The relatively few children who are hard of hearing and deaf and who have had the benefit of an effective EHDI system demonstrate gains in language not commonly reported. Only when language and literacy performance data are available for a generation of children with hearing loss who received the benefit of early detection and intervention will the true cost of EHDI be known. When outcomes for infants and their families are compared to the costs of these services, the community can judge the value of EHDI.
References
Agency for Health Care Policy and Research. (1995). Using clinical practice guidelines to evaluate quality of care (Vol. 2, Methods, AHCPR Pub. No. 95-0046). Washington, DC: U.S. Department of Health and Human Services Public Health Service.
American Academy of Audiology. (1998). Draft: Use of support personnel for newborn hearing screening. Audiology Today, 21-23.
American Academy of Pediatrics. (1992). Ad hoc task force on definition of the medical home. Pediatrics, 90, 5 (RE9262).
American Academy of Pediatrics. (1993, November). The medical home statement addendum. American Academy of Pediatrics News.
American Academy of Pediatrics. (1999a). Privacy protection of health information: Patient rights and pediatrician responsibilities. Pediatrics, 104, 973-977.
American Academy of Pediatrics. (1999b). Newborn and infant hearing loss: Detection and Intervention. Task Force on Newborn and Infant Hearing. Pediatrics, 103, 527-530.
American Speech-Language-Hearing Association. (1989). Communication-based services for infants, toddlers, and their families. Asha, 31, 32-34, 94.
American Speech-Language-Hearing Association. (1997). Guidelines for audiologic screening. Rockville, MD: ASHA.
American Speech-Language-Hearing Association, American Academy of Audiology, & Alexander Graham Bell Association for the Deaf. (1997). A Model Universal Newborn/Infant Hearing Screening, Tracking, and Intervention Bill. Rockville, MD: ASHA.
American Speech-Language-Hearing Association. (1991). The use of FM amplification instruments for infants and preschool children with hearing impairment. Asha, 33,(Suppl.5), 1-2.
Arehart, K. H., Yoshinaga-Itano, C., Thomson, V., Gabbard, S. A., & Stredler Brown, A. (1998). State of the States: The status of universal newborn screening, assessment, and intervention systems in 16 States. American Journal of Audiology, 7, 101-114.
Baker-Hawkins, S., & Easterbrooks, S. (Eds.). (1994). Deaf and hard of hearing students: Educational service delivery guidelines. Alexandria, VA: National Association of State Directors of Special Education.
Bamford, J. M. (1998). Early intervention: what then? In F. H. Bess (Ed.), Children with hearing impairment: Contemporary trends, (pp. 353-370). Nashville, TN: The Vanderbilt Bill Wilkerson Center Press.
Berlin, C. I., Bordelon, J., St. John, P., Wilensky, D., Hurley, A., Kluka, E., & Hood, L. J. (1999). Reversing click polarity may uncover auditory neuropathy in infants. Ear and Hearing, 19(1), 37-47.
Bess, F. H. (1998). Children with hearing impairment: Contemporary trends. Nashville, TN: Vanderbilt Bill Wilkerson Center Press.
Bess, F. H., Dodd-Murphy, J., & Parker, R. A. (1998). Children with minimal sensorineural hearing loss: Prevalence, educational performance, and functional status. Ear and Hearing, 19, 339-354.
Bess, F. H., & McConnell, F. E. (1981). Audiology education and the hearing impaired child. St. Louis: C. V. Mosby Company.
Bess, F. H., & Tharpe, A. M. (1984). Unilateral hearing impairment in children. Pediatrics, 74, 206-216.
Bess, F. H., & Tharpe, A. M. (1986). An introduction to unilateral sensorineural hearing loss in children. Ear and Hearing, 7(1), 3-13.
Blair, J. C., Peterson, M. E., & Vieweg, S. H. (1985). The effects of mild sensorineural hearing loss on academic performance of young school-age children. The Volta Review, 87(2), 87-93.
Brick, K. (1999, June 7). Genetics of deafness, deaf people and the past, present and future. Workshop on the Genetics of Congenital Hearing Impairment. Centers for Disease Control and Prevention and Gallaudet University, Atlanta, GA.
Brookhouser, P., Worthington, D., & Kelly, W. (1994). Fluctuating and or progressive sensorineural hearing loss in children. Laryngoscope, 104, 958-964.
Calderon, R., Bargones, J., & Sidman, S. (1998). Characteristics of hearing families and their young deaf and hard of hearing children: Early intervention follow-up. American Annals of the Deaf, 143, 347-362.
Carney, A., and Moeller, M. P. (1998). Treatment efficacy: Hearing loss in children. Journal of Speech and Hearing Research, 41, S61-S84.
Carpenter, C., Bender, A. D., Nash, D. B., & Cornman, J. C. (1996). Must we choose between quality and cost containment? Quality in Health Care, 5, 223-229.
Centers for Disease Control and Prevention. (1997, November 14). Serious hearing impairment among children aged 3-10 years–Atlanta, GA, 1991-1993. Morbidity and Mortality Weekly Report.
Cherow, E., Dickman, D., & Epstein, S. (1999). Organization resources for families of children with deafness or hearing loss. In N. J. Roizen & A. O. Diefendorf (Eds.), Pediatric Clinics of North America, 46, 153-162.
Cherow, E., Matkin, N. D., & Trybus, R. (Eds.). (1985). Hearing impaired children and youth with developmental disabilities: An interdisciplinary foundation for service. Washington, DC: Gallaudet University Press.
Christensen, K. M., & Delgado, G. L. (1993). Multicultural issues in deafness. White Plains, NY: Longman Publishing Group.
Clark, T. (1993). SKI*HI: Applications for home-based intervention. In J. Roush and N. D. Matkin (Eds.), Infants and toddlers with hearing loss: Family centered assessment and intervention (pp. 237-251). Baltimore, MD: York Press, Inc.
Cohen, O. P. (1997). Giving all children a chance: Advantages of an anti-racist approach to education for deaf children. American Annals of the Deaf, 142(2), 80-82.
Cohen, O. P. (1993). Educational needs of the African-American and Hispanic deaf children and youth. In K. M. Christensen & G. L. Delgado (Eds.), Multicultural issues in deafness (pp. 45-57). White Plains, NY: Longman Publishing Group.
Cohen, O. P., Fischgrund, J., & Redding, R. (April, 1990). Deaf children from ethnic and racial minority backgrounds: An overview. American Annals of the Deaf, 135, 67-73.
Cohn, E., Kelley, P., Fowler, T., Gorga, M., Lefkowitz, D., Kuehn, H., Schaefer, G. B., Gobar, L., Hahn, F., Harris, D., & Kimberling, W. (1999). Clinical studies of families with hearing loss attributable to mutations in the connexin 26 gene (GJB2/DFNB1). Pediatrics, 103, 546-550.
Cone-Wesson, B., & Ramirez, G. M. (1997). Hearing sensitivity in newborns estimated from ABRs to bone-conducted sounds. Journal of the American Academy of Audiology, 8, 299-307.
Cone-Wesson, B., Vohr, B. R., Sininger, Y. S., Widen, J. E., Folsom, R. C., Gorga, M. P., & Norton, S. J. (in press). Identification of neonatal hearing impairment: Infants with hearing impairment. Ear and Hearing.
Corley, V., & Crabbe, L. (1999). Auditory neuropathy and a mitochondrial disorder in a child: A case study. Journal of the American Academy of Audiology, 10, 484-488.
Dalzell, L., Orlando, M., MacDonald, M., Berg, A., Bradley, M., Cacace, A., Campbell, D., DeCristofaro, J., Gravel, J., Greenberg, E., Gross, S., Pinheiro, J., Regan, J., Spivak, L., Stevens, F., & Prieve, B. (2000). The New York State universal newborn hearing screening demonstration project: Ages of hearing loss identification, hearing aid fitting and enrollment in early intervention. Ear and Hearing, 21, 118-130.
Davis, J., Elfenbein, J., Schum, R., & Bentler, R. (1986). Effects of mild and moderate hearing impairment on language, educational and psychosocial behavior of children. Journal of Speech and Hearing Disorders, 51, 53-62.
Davis, J., Shepard, N. T., Stelmachowicz, P. G., & Gorga, M. P. (1981). Characteristics of hearing-impaired children in the public schools: Pt. II–Psychoeducational data. Journal of Speech and Hearing Disorders, 46, 130-137.
Demmler, G. (1991). Infectious Diseases Society of America and Centers for Disease Control. Summary of a workshop on surveillance for congenital cytomegalovirus disease. Review of Infectious Diseases, 13, 315-329.
Denoyelle F., Marlin, S., Weil, D., Moatti, L., Chauvin, P., Garabedian, E. N., & Petit, C. (1999, April 17). Clinical features of the prevalent form of childhood deafness, DFNB1, due to a connexin-26 gene defect: Implications for genetic counseling. Lancet, 353, 1298-1303.
Diefendorf, A. O., & Finitzo, T. (1997). The state of the information. American Journal of Audiology, 6, 73.
Diefendorf, A. O., & Gravel, J. S. (1996). Behavioral observation and visual reinforcement audiometry. In S. Gerber (Ed.), Handbook of pediatric audiology (pp. 55-83). Washington, DC: Gallaudet University Press.
Doyle, K., Burggraaff, B., Fujikawa, S., Kim, J., & MacArthur, C. (1997). Neonatal hearing screening with otoscopy, auditory brainstem response and otoacoustic emissions.Otolaryngology–Head and Neck Surgery, 116, 597-603.
Eilers, R., Miskiel, E., Ozdamar, O., Urbano, R., & Widen, J. E. (1991). Optimization of automated hearing test algorithms: Simulations using an infant response model. Ear and Hearing, 12, 191-198.
Elssmann, S. A., Matkin, N. D., & Sabo, M. P. (1987, Sept.). Early identification of congenital sensorineural hearing impairment. The Hearing Journal, 40(9), 13-17.
Finitzo, T. (1999). The Sounds of Texas project: Principles from the 1994 Joint Committee on Infant Hearing Position Statement. In F. Grandori & M. Lutman, (Eds.), The European Consensus Statement on Neonatal Hearing Screening (pp. 38-43). Milan, Italy.
Finitzo, T., Albright, K., & O'Neal, J. (1998). The newborn with hearing loss: Detection in the nursery. Pediatrics, 102, 1452-1460.
Finitzo-Hieber, T., McCracken, G., & Brown, K. (1985). Prospective controlled evaluation of auditory function in neonates given netilmicin or amikacin. Pediatrics, 106, 129-135.
Fisher, R. M. (1994). The Mama Lere Home. In J. Roush & N. D. Matkin (Eds.), Infants and toddlers with hearing loss: Family centered assessment and intervention (pp. 195-213). Baltimore, MD: York Press, Inc.
Fletcher, R. H., Fletcher, S. W., & Wagner E. W. (1988). Clinical epidemiology: The essentials. (2nd ed.). Baltimore, MD: Williams & Wilkins.
Fortnum, H., & Davis, A. (1997). Epidemiology of permanent childhood hearing impairment in Trent Region, 1985-1993. British Journal of Audiology, 31, 409-446.
Friel-Patti, S., & Finitzo, T. (1990). Language learning in a prospective study of otitis media with effusion. Journal of Speech Hearing Research, 33, 188-194.
Friel-Patti, S., Finitzo, T., Meyerhoff, W., & Hieber, J. (1986). Speech-language learning and early middle ear disease: A procedural report. In J. Kavanaugh (Ed.), Otitis media and child development (pp. 129-138). Parkton, MD: York Press.
Friel-Patti, S., Finitzo-Hieber, T., Conti, G., & Brown, K. C. (1982). Language delay in infants associated with middle ear disease and mild, fluctuating hearing impairment.Pediatric Infectious Diseases, 1(2), 104-109.
Gallaudet University Center for Assessment and Demographic Study. (1998). Thirty years of the annual survey of deaf and hard of hearing children and youth: A glance over the decades. American Annals of the Deaf, 142(2), 72-76.
Glattke, T. J., Pafitis, I. A., Cummiskey, C., & Herer, G. R. (1995). Identification of hearing loss in children using measures of transient otoacoustic emission reproducibility.American Journal of Audiology, 4(3), 71-86.
Goldberg, D. M., & Flexer, C. (1993). Outcome survey of auditory-verbal graduates: Study of clinical efficacy. Journal of the American Academy of Audiology, 4, 189-200.
Gorga, M., Neely, S., Bergman, B., Beauchaine, K., Kaminski, J., Peters, J., & Jesteadt, W. (1993). Otoacoustic emissions from normal-hearing and hearing-impaired subjects: Distortion product responses. Journal of the Acoustical Society of America, 93, 2050-2060.
Gravel, J. S., & Wallace, I. F. (1992). Listening and language at 4 years of age: Effects of early otitis media. Journal of Speech and Hearing Research, 35, 588-595.
Gravel, J. S., & Stapells, D. R. (1993). Behavioral, electrophysiologic, and otoacoustic measures from a child with auditory processing dysfunction: Case report. Journal of the American Academy of Audiology, 4, 412-419.
Gravel, J. S., & Hood, L. J. (1999). Pediatric audiologic assessment. In F. E. Musiek & W. F. Rintelmann (Eds.), Contemporary perspectives in hearing assessment (pp. 305-326). Boston: Allyn & Bacon.
Gravel, J., Berg, A., Bradley, M., Cacace, A., Campbell, D., Dalzell, L., DeCristofaro, J., Greenberg, E., Gross, S., Orlando, M., Pinheiro, J., Regan, J., Spivak, L., Stevens, F., & Prieve, B. (2000). The New York State universal newborn hearing screening demonstration project: Effects of screening protocol on inpatient outcome measures. Ear and Hearing, 21, 131-140.
Green, G. E., Scott, D. A., McDonald, J. M., Woodworth, G. G., Sheffield, V. C., & Smith, R. J. (1999). Carrier rates in the Midwestern United States for GJB2 mutations causing inherited deafness. Journal of the American Medical Association, 281, 2211-2216.
Guralnick, M. J. (1997). Second generation research in the field of early intervention. In M. Guralnick (Ed.), The effectiveness of early intervention (pp. 3-20). Baltimore: Paul H. Brookes.
Harrison, M., & Roush, J. (1996). Age of suspicion, identification and intervention for infants and young children with hearing loss: A national study. Ear and Hearing, 17, 55-62.
Hayes, D. (1999). State programs for universal newborn hearing screening. In N. J. Roizen & A. O. Diefendorf (Eds.), Pediatric Clinics of North America, 46, 89-94.
Herrmann, B., Thornton, A., & Joseph, J. (1995). Automated infant screening using the ABR: Development and evaluation. American Journal of Audiology, 4, 6-14.
Hyde, M., Davidson, M. J., and Alberti, P. W. (1991). Auditory test strategy. In J. T. Jacobsen & J. L. Northern (Eds.), Diagnostic audiology (pp. 295-322). Austin, TX: Pro-Ed.
Hyde, M. L., Riko, K., & Malizia, K. (1990)., Audiometric accuracy of the click ABR in infants at risk for hearing loss. Journal of the American Academy of Audiology, 1, 59-66.
Hyde, M. L., Sininger, Y. S., & Don, M. (1998). Objective detection and analysis of ABR: An historical perspective. Seminars in Hearing, 19, 97-113.
Individuals with Disabilities Education Act Amendments of 1997. P. L. No. 105-17,111, Stat. 38 (1997). Codified as amended at 20 U. S. C. Section 1400-1485.
Infant Health and Development Program. (1990). Enhancing the outcomes of low-birth-weight, premature infants. Journal of the American Medical Association, 263, 3035-3042.
Jerger, J., & Hayes, D. (1976). The cross-check principal in pediatric audiology. Archives of Otolaryngology, 102, 614-620.
Jerger, S., Jerger, J., Alford, B. R, & Abrams, S. (1983). Development of speech intelligibility in children with recurrent otitis media. Ear and Hearing, 4, 138-145.
Johnson, D. (1999). Deafness and vision disorders: Anatomy and physiology, assessment procedures, ocular anomalies and educational implications. Springfield, IL: Charles Thomas, Publisher.
Joint Committee of the American Speech-Language-Hearing Association and the Council on Education of the Deaf. (1994, August). Service provision under the Individuals with Disabilities Education Act–Part H, as Amended, to children who are deaf and hard of hearing ages birth to 36 months. Asha, 36, 117-121.
Joint Committee on Infant Hearing. (1994a). Joint Committee on Infant Hearing 1994 Position Statement. AAO-HNS Bulletin, 13, 12.
Joint Committee on Infant Hearing. (1994b, December). Joint Committee on Infant Hearing. (1994). Position Statement. Asha, 36, 38-41.
Joint Committee on Infant Hearing. (1995a). Joint Committee on Infant Hearing 1994 Position Statement. Audiology Today, 6, 6-9.
Joint Committee on Infant Hearing. (1995b). Joint Committee on Infant Hearing 1994 Position Statement. Pediatrics, 95, 315.
Karchmer, M., & Allen, T. (1999). The functional assessment of deaf and hard of hearing students. American Annals of the Deaf, 144, 68-77.
Keefe, D. H., & Levi, E. (1996). Maturation of the middle ear and external ears: Acoustic power-based responses and reflectance tympanometry. Ear and Hearing, 17, 361-373.
Kile, J. (1993). Identification of hearing impairment in children: A 25-year review. The Transdisciplinary Journal, 3(3), 155-164.
Khoury, M. (1999). What happens after a gene is found? Population research to use genetic information to improve health and prevent disease. Presented at the Workshop on the Genetics of Congenital Hearing Impairment: Centers for Disease Control and Prevention and Gallaudet University, Atlanta, GA.
Kraus, N., Ozdamar, O., Stein, L., & Reed, N. (1984). Absent auditory brain stem response: Peripheral hearing loss or brain stem dysfunction? Laryngoscope, 94, 400-406.
Kuhl, P. K., Williams, K. A., Lacerda, F., Stevens, K. N., & Lindblom, B. (1992). Linguistic experience alters phonetic perception in infants by 6 months of age. Science, 255, 606-608.
Kuhl, P., Andruski, J., Chistovich, I., Chistovich, L., Kozhevnikova, E., Ryskina, V., Stolyarova, E., Sundberg, U., & Lacerda, F. (1997). Cross-language analysis of phonetic units in language addressed to infants. Science, 277, 684-686.
Littman, T., Demmler, G., Williams, S., Istas, A., & Griesser, C. (1995). Congenital asymptomatic cytomegalovirus infection and hearing loss. Abstracts for the Association for Research in Otolaryngology, 19, 40.
Luterman, D. (1985). The denial mechanism. Ear and Hearing, 6(1), 57-58.
Luterman, D., & Kurtzer-White, E. (1999). Identifying hearing loss: Parents' needs. American Journal of Audiology, 8, 8-13.
Mahshie, S. N. (1995). Educating deaf children bilingually. Washington, DC: Gallaudet University Press.
Marchant, C. D., McMillan, P. M., Shurin, P. A., Johnson, C. E., Turczyk, V. A., Feinstein, J. C., & Panek, D. M. (1986). Objective diagnosis of otitis media in early infancy by tympanometry and ipsilateral acoustic reflex thresholds. Journal of Pediatrics, 109, 590-595.
Marschark, M. (1997). Raising and educating a deaf child. New York: Oxford University Press.
Mason, J., & Hermann, K. R. (1998). Universal infant hearing screening by automated auditory brainstem response measurement. Pediatrics, 101, 221-228.
Matkin, N. D. (1988). Key considerations in counseling parents of hearing impaired children. Seminars in Hearing, 209-222.
McFarland, W., Simmons, F., & Jones, F. (1980). An automated hearing screening technique for newborns. Journal of Speech and Hearing Disorders, 45, 495.
Meadow-Orleans, K. P., Mertens, D. M., Sass-Lehrer, M., & Scott-Olson, K. (1997). Support services for parents and their children who are deaf or hard of hearing. American Annals of the Deaf, 142, 278-288.
Mehl, A. L., & Thomson, V. (1998). Newborn hearing screening: The great omission. Pediatrics, 101, e4.
Moeller, M. P., & Condon, M. (1994). A collaborative, problem-solving approach to early intervention. In J. Roush & N. D. Matkin (Eds.), Infants and toddlers with hearing loss: Identification, assessment and family-centered intervention (pp. 163-192). Parkton, MD: York Press Inc.
Moeller, M. P. (2000, in press). Early intervention and language development in children who are deaf and hard of hearing. Pediatrics.
Moses, K. (1985). Dynamic intervention with families. In E. Cherow, N. D. Matkin, & R. Trybus (Eds.), Hearing impaired children and youth with developmental disabilities: An interdisciplinary foundation for service (pp. 82-98). Washington, DC: Gallaudet University Press.
Morton, C. (1999, June 7). The NIDCD Working Group on genetic testing for deafness and other communication disorders: Considerations for developing and implementing testing. Presented at Workshop on the Genetics of Congenital Hearing Impairment: Centers for Disease Control and Prevention and Gallaudet University, Atlanta, GA.
National Institute on Deafness and other Communication Disorders. (1993, March 1-3). National Institutes of Health Consensus Statement: Early identification of hearing impairment in infants and young children. Bethesda, MD: Author. http://odp.od.nih.gov/consensus/cons/092/092 intro.htm
National Institute on Deafness and other Communication Disorders. (1997). Recommendations of the NIDCD Working Group on Early Identification of Hearing Impairment on acceptable protocols for use in state-wide universal newborn hearing screening programs. Bethesda, MD: NIDCD Clearing House ([email protected])
National Institute on Deafness and other Communication Disorders. (1998, Feb. 2-3). Economic and social realities of communication differences and disorders: Fact finding report. Bethesda, MD: Author.
National Institute on Deafness and Other Communication Disorders. (1999, September). Communicating informed consent to individuals who are Deaf or hard-of-hearing(DHHS, NIH Pub No. 00-4689). Bethesda, MD: Author.
Norton, S. J., Gorga, M. P. Widen, J. E., Folsom, R. C., Sininger, Y. S., Cone-Wesson, B., Vohr, B. R., & Fletcher, K. (in press). Identification of neonatal hearing impairment: A multi-center investigation. Ear and Hearing.
O'Donnell, N. S., & Galinsky, E. (1998). Measuring progress and results in early childhood system development. New York: Families and Work Institute. www.familiesandwork.org.
Ogden, P. (1996). The silent garden. Washington, DC: Gallaudet University Press.
O'Neal, J. (1997). From description to definition: Avoiding a tower of babel. American Journal of Audiology, 6, 73.
Oyler, R. F., Oyler, A. L., & Matkin, N. D. (1988). Unilateral hearing loss demographic and educational impact. Language, Speech, and Hearing Services in Schools, 19, 191-200.
Ozdamar, O., Kraus, N., & Stein, L. (1983). Auditory brainstem responses in infants recovering from bacterial meningitis. Archives of Otolaryngology–Head and Neck Surgery, 109,13-18.
Ozdamar, O., Delgado, R. E., Eilers, R. E., & Urbano R. C. (1994). Automated electrophysiologic hearing testing using a threshold-seeking algorithm. Journal of the American Academy of Audiology, 5(2), 77-88.
Pediatric Working Group of the Conference on Amplification for Children with Auditory Deficits. (1996). Amplification for infants and children with hearing loss. American Journal of Audiology, 5(1), 53-68.
Pollack, D., Goldberg, D., & Coleffe-Schenck, N. (1997). Educational audiology for the limited-hearing infant and preschooler: An auditory verbal program (3rd ed.). Springfield, IL: Charles Thomas, Publisher.
Pool, K., & Finitzo, T. (1989). A computer-automated program for clinical assessment of the auditory brain stem response. Ear and Hearing, 10, 304-310.
Pool, K. D. (1996). Infant hearing detection programs: Accountability and information management. Seminars in Hearing, 17, 139-151.
Prieve, B., Gorga, M., Schmidt, A., Neely, S., Peters, J., Schulte, L., & Jesteadt, W. (1993). Analysis of transient-evoked otoacoustic emissions in normal-hearing and hearing-impaired ears. Journal of the Acoustical Society of America, 93, 3308-3319.
Prieve, B. A., Fitzgerald, T. S., Schulte, L. E., & Demp, D. T. (1997). Basic characteristics of distortion product otoacoustic emissions in infants and children. Journal of the Acoustical Society of America, 102, 2871-2879.
Prieve, B., Dalzell, L., Berg, A., Bradley, M., Cacace, A., Campbell, D., DeCristofaro, J., Gravel, J., Greenberg, E., Gross, S., Orlando, M., Pinheiro, J., Regan, J., Spivak, L., & Stevens, F. (2000). The New York State universal newborn hearing screening demonstration project: Outpatient outcome measures. Ear and Hearing, 21, 104-117.
Prieve, B., & Stevens, F. (2000). The New York State universal newborn hearing screening demonstration project: Introduction and overview. Ear and Hearing, 21, 85-91.
Psarommatis, I. M., Tsakanikos, M. D., Kontorgianni, A. D., Ntourniadakis, D. E., & Apostolopoulos, N. K. (1997). Profound hearing loss and presence of click-evoked otoacoustic emissions in the neonate: A report of two cases. International Journal of Pediatric Otorhinolaryngology, 39, 237-243.
Ramey C., & Ramey, S. L. (1992). Early intervention with disadvantaged children–To what effect? Appl. Prev Psychol, 1, 131-140.
Ramey, C., & Ramey, S. L. (1998). Prevention of intellectual disabilities: Early interventions to improve cognitive development. Preventive Medicine, 27, 224-232.
Rance, G., Beer, D. E., Cone-Wesson, B., Shepard, R. K., Dowell, R. C., King, A. M., Rickards, F. W., & Clark, G. M. (1999). Clinical findings for a group of infants and young children with auditory neuropathy. Ear and Hearing, 20(3), 238-252.
Rance, G., Rickards, F. W., Cohen, L. T., DeVidi, S., & Clark, G. M. (1995). The automated prediction of hearing thresholds in sleeping subjects using auditory steady state evoked potentials. Ear and Hearing, 16, 499-507.
Roberts, J. E., Burchinal, M. R., Medley, L. P., Zeisel, S. A., Mundy, M., Roush, J., Hooper, S., Bryant, D., & Henderson, F. W. (1995). Otitis media, hearing sensitivity, and maternal responsiveness in relation to language during infancy. Journal of Pediatrics, 126, 481-489.
Roizen, N. J. (1999). Etiology of hearing loss in children: Nongenetic causes. Pediatric Clinics of North America, 46(1), 49-64.
Ross, M. (1990). Implications of delay in detection and management of deafness. Volta Review, 92(2), 69-79.
Roush, J., & Matkin, N. D. (Eds.). (1994). Infants and toddlers with hearing loss: Family-centered assessment and intervention. Baltimore: York Press.
Rushmer, N. (1992). Parent-infant intervention strategies: A focus on relationships. In F. H. Bess & J. W. Hall III (Eds.). Screening children for auditory function (pp. 463-476). Nashville, TN: Bill Wilkerson Center Press.
Sackett, D. L., Haynes, R. B., & Tugwell, P. (1991). Clinical epidemiology: A basic science for clinical medicine (2nd ed.). Boston: Little, Brown and Company.
Schildroth, A. N., & Hotto, S. A. (1993). Annual survey of hearing-impaired children and youth: 1991-1992 school year. American Annals of the Deaf, 138(2), 163-171.
Schwartz, S. (1996). Choices in deafness: A parent's guide to communication options (2nd ed.). Bethesda, MD: Woodbine House.
Scott, D. M. (1998). Multicultural aspects of hearing disorders and audiology. In D. E. Battle (Ed.). Communication disorders in multicultural populations (2nd ed., pp. 335-354). Boston: Butterworth-Heinemann.
Sininger, Y. S., Abdala, C., & Cone-Wesson, B. (1997). Auditory threshold sensitivity of the human neonate as measured by the auditory brainstem response. Hearing Research, 104, 27-38.
Sininger, Y. S., Doyle, K. J., & Moore, J. K. (1999). The case for early identification of hearing loss in children. In N. J. Roizen & A. O. Diefendorf (Eds.). Pediatric Clinics of North America, 46, 1-13.
Sininger, Y. S., Hood, L. J., Starr, A., Berlin, C. I. and Picton, T. W. (1995). Hearing loss due to auditory neuropathy. Audiology Today, 7, 10-13.
Spivak, L. (1998). Universal newborn hearing screening. New York: Thieme.
Spivak, L., Dalzell, L., Berg, A., Bradley, M., Cacace, A., Campbell, D., DeCristofaro, J., Gravel, J., Greenberg, E., Gross, S., Orlando, M., Pinheiro, J., Regan, J., Stevens, F., & Prieve, B. (2000). The New York State universal newborn hearing screening demonstration project: Inpatient outcome measures. Ear and Hearing, 21, 92-103.
Stapells, D. R., Gravel, J. S., & Martin, B. A. (1995). Thresholds for auditory brainstem responses to tones in notched noise from infants and young children with normal hearing or sensorineural hearing loss. Ear and Hearing, 16(4), 361-371.
Starr, A., Picton, T. W., Sininger, Y., Hood, L. J., & Berlin, C. I. (1996). Auditory neuropathy. Brain, 119, 741-753.
Stein, L., Tremblay, K., Pasternak, J., Banerjee, S., Lindemann, K., & Kraus, N. (1996). Brainstem abnormalities in neonates with normal otoacoustic emissions. Seminars in Hearing, 17, 197-213.
Stelmachowicz, P. G. (1999). Hearing aid outcome measures for children. Journal of the American Academy of Audiology, 10(1), 14-25.
Stool, S. E., Berg, A. O., Berman, S., Carney, C. J., Cooley, J. R., Culpepper, L., Eavey R. D., Feagans, L. V., Finitzo, T., Friedman, E., et. al. (1994). Managing otitis media with effusion in young children. Quick reference guide for clinicians (AHCPR Publication 94-0623). Rockville, MD: Agency for Health Care Policy and Research, Public Health Service, U. S. Department of Health and Human Services.
Stredler-Brown, A., & Yoshinaga-Itano, C. (1994). Family assessment: A multidisciplinary evaluation tool. In J. Roush & N. D. Matkin (Eds.). Infants and toddlers with hearing loss. Baltimore, MD: York Press, Inc.
Stredler-Brown, A. (1998). Early intervention for infants and toddlers who are deaf and hard of hearing: New perspectives. Journal of Educational Audiology, 6, 45-49.
Tharpe, A. M., & Clayton, E. W. (1997). Newborn hearing screening: Issues in legal liability and quality assurance. American Journal of Audiology, 6, 5-12.
Tharpe, A. M., & Bess, F. H. (1999). Minimal, progressive, and fluctuating hearing losses in children: Characteristics, identification, and management. In N. J. Roizen and A. O. Diefendorf (Eds.), Pediatric Clinics of North America, 46(1), 65-78.
Thomblin, J. B., Spencer, L., Flock, S., Tyler, R., & Gantz, B. (1999). A comparison of language achievement in children with cochlear implants and children using hearing aids.Journal of Speech, Language, and Hearing Research, 42, 497-511.
Thompson, M. (1994). ECHI. In J. Roush & N. D. Matkin (Eds.). Infants and toddlers with hearing loss: Family centered assessment and intervention (pp. 253-275). Baltimore, MD: York Press, Inc.
Tomaski, S., & Grundfast, K. (1999). A stepwise approach to the diagnosis and treatment of hereditary hearing loss. In N. J. Roizen & A. O. Diefendorf (Eds.), Pediatric Clinics of North America, 46(1), 35-48.
U.S. Department of Education, Office of Special Education and Rehabilitative Services. (1998, Apr. 14). Final regula-tions: Early intervention program for infants and toddlers with disabilities. Federal Register (34 CFR Pt. 303).
U.S. Department of Health and Human Services. (2000). Healthy People 2010 (Conference ed., in Two Volumes). Washington, DC: January 2000
U.S. Department of Health and Human Services Public Health Service. (1990). Healthy People 2000, National health promotion and disease prevention objectives for the nation(DHHS Publication No. (PHS) 91-50212). Washington, DC: U.S. Government Printing Office.
Vohr, B. R., Carty, L., Moore P., & Letourneau, K. (1998). The Rhode Island Hearing Assessment Program: Experience with statewide hearing screening (1993-1996). Journal of Pediatrics, 133, 353-357.
Vohr, B. R., & Maxon, A. (1996). Screening infants for hearing impairment. Journal of Pediatrics, 128, 710-714.
Vohr, B. R., Widen, J. E., Cone-Wesson, B., Sininger, Y. S., Gorga, M. P., Folsom, R. C., & Norton, S. J. (in press). Identification of neonatal hearing impairment: Characteristics of infants in the neonatal intensive care unit (NICU) and well baby nursery. Ear and Hearing.
Wallace, I. F., Gravel, J. S., Ruben, R. J., McCarton, C. M., Stapells, D., & Bernstein, R. S. (1988). Otitis media, language outcome and auditory sensitivity. Laryngoscope, 98,64-70.
Wheeler, D. J., & Chambers, D. S. (1986). Understanding statistical process control. Knoxville, TN: SPC Press, Inc.
White, K. R. & Maxon, A. B. (1999). Early identification of hearing loss: Implementing universal newborn hearing screening programs (MCHK125). Vienna, VA: National Maternal and Child Health Clearinghouse.\\ Williamson, W. D., Demmler, G. J., Percy, A. K., & Catlin, F. I. (1992). Progressive hearing loss in infants with asymptomatic congenital cytomegalovirus infection. Pediatrics, 90, 862-866.
Yoshinaga-Itano, C. (1995). Efficacy of early identification and intervention. Seminars in Hearing, 16, 115-120.
Yoshinaga-Itano, C., Sedey, A., Coulter, D. K., & Mehl, A. L. (1998). Language of early and later identified children with hearing loss. Pediatrics, 102, 1161-1171.





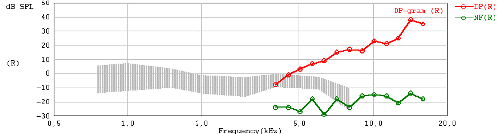










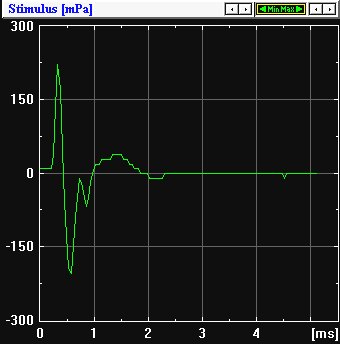 Figure 1: Ideal shape of a click TEOAE stimulus
Figure 1: Ideal shape of a click TEOAE stimulus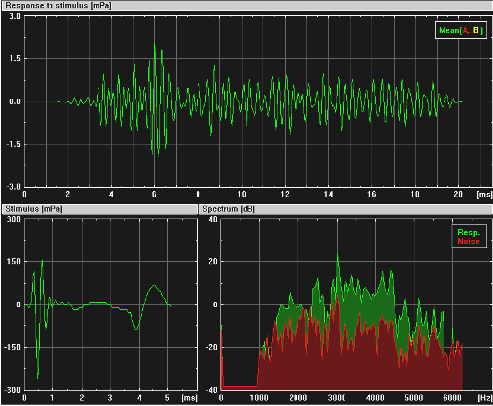







































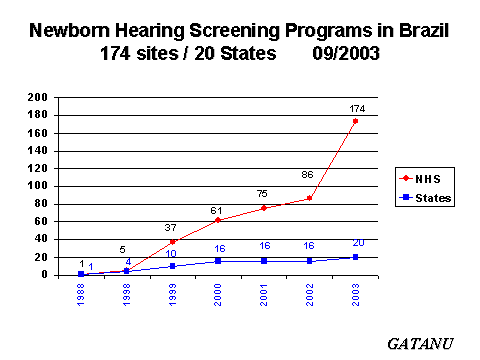
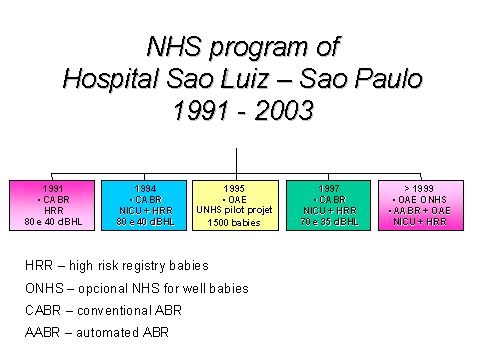





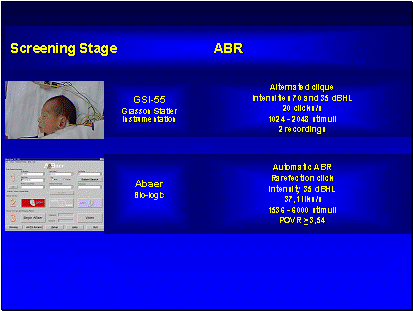


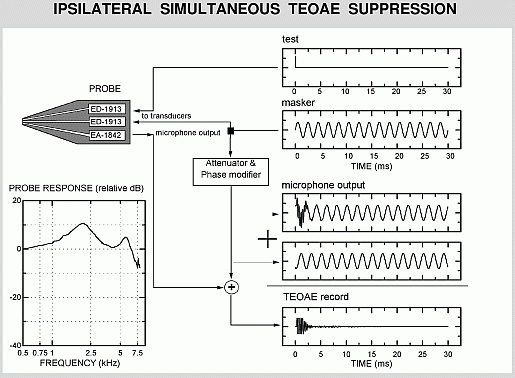
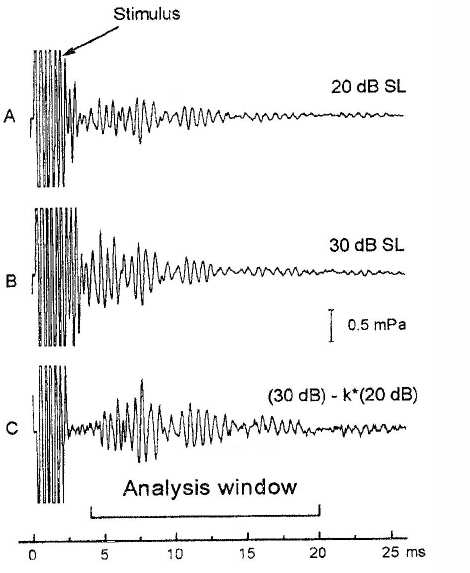
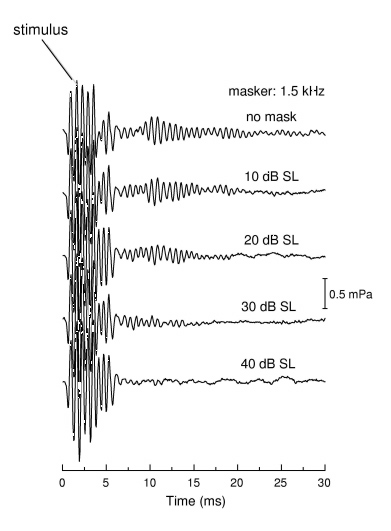
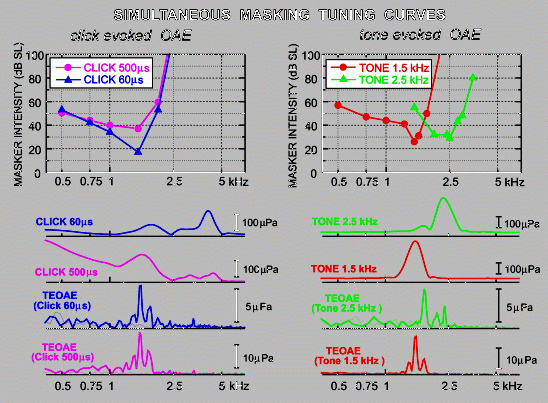
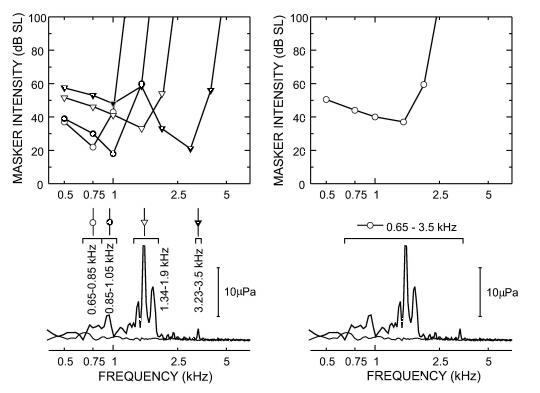
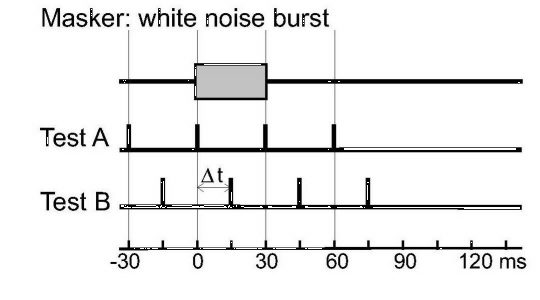
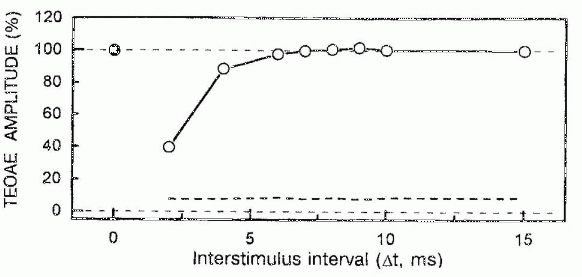
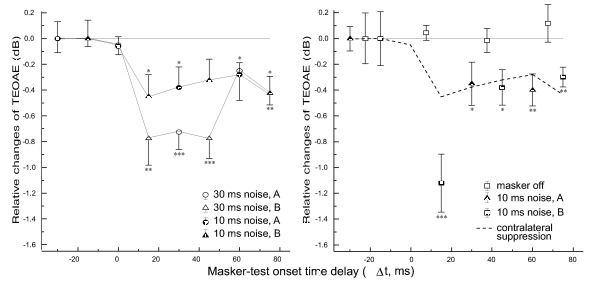
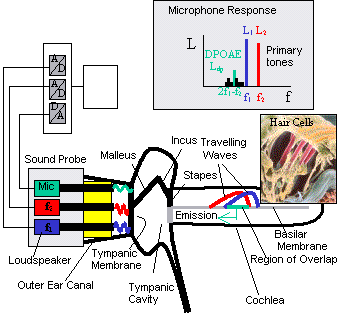
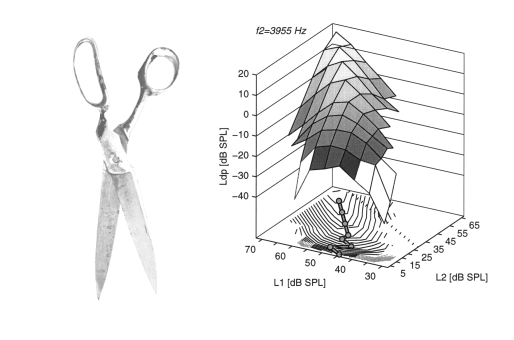
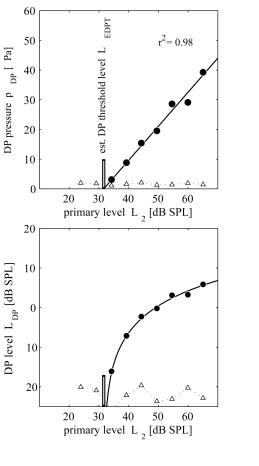
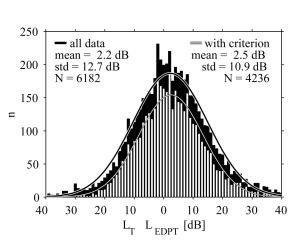
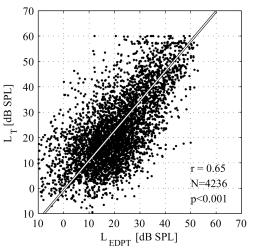








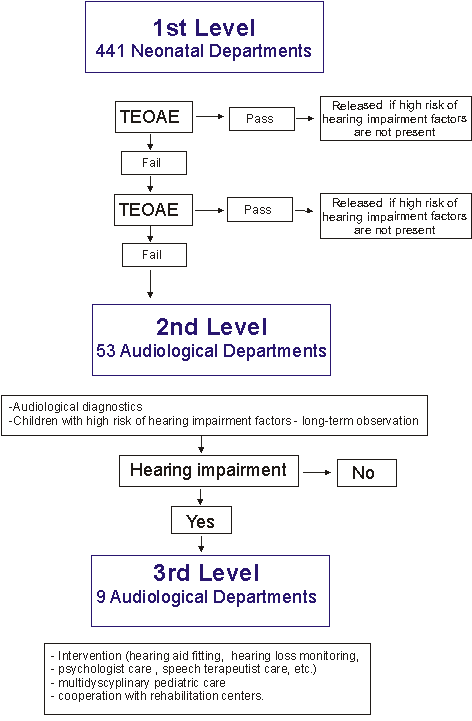
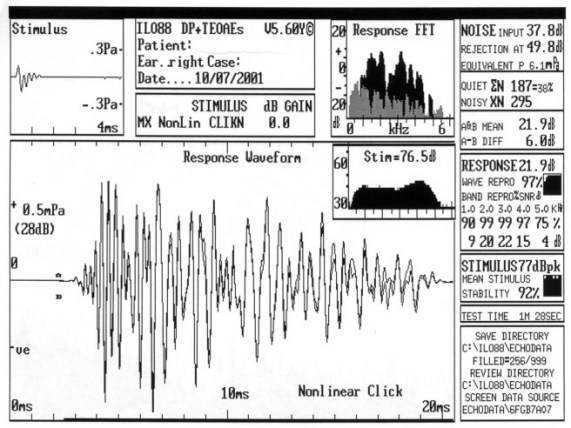
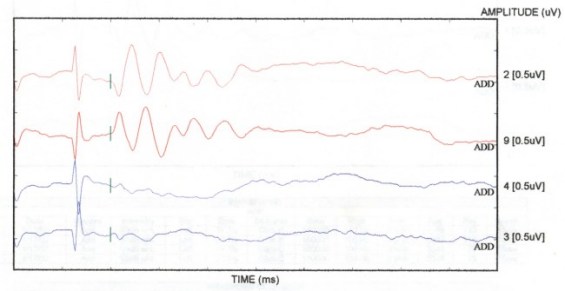
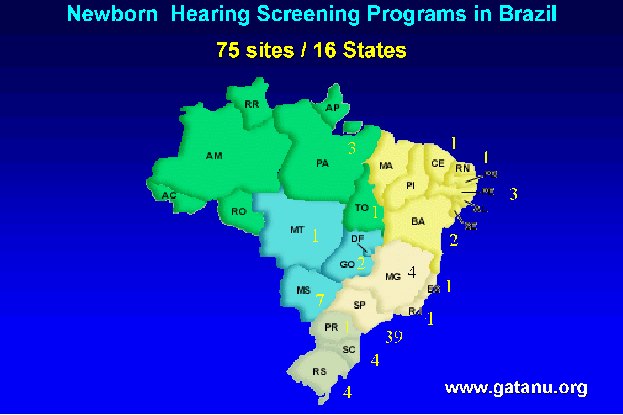


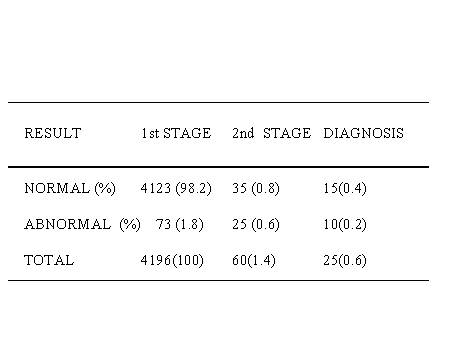
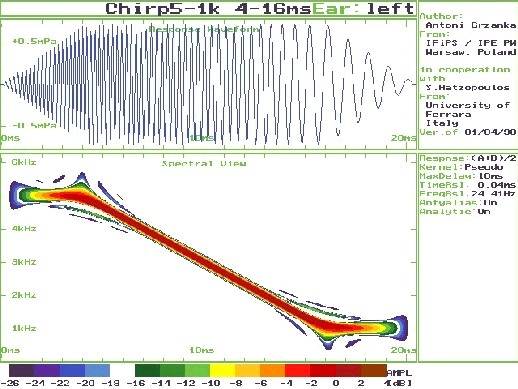
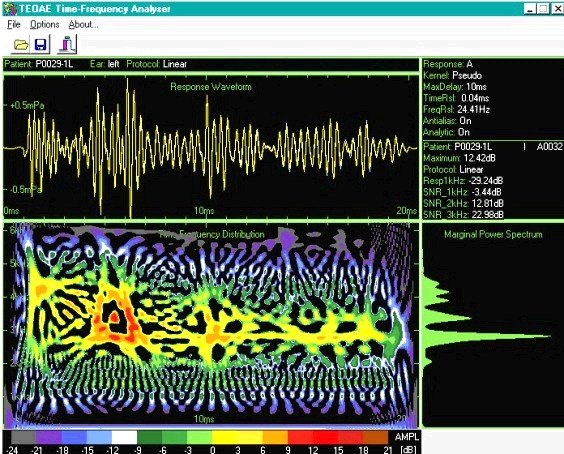
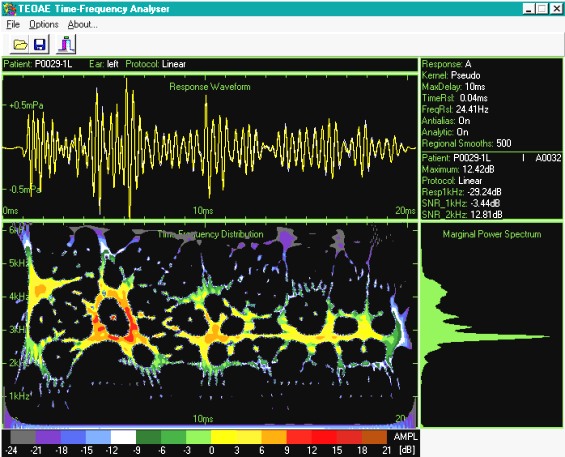
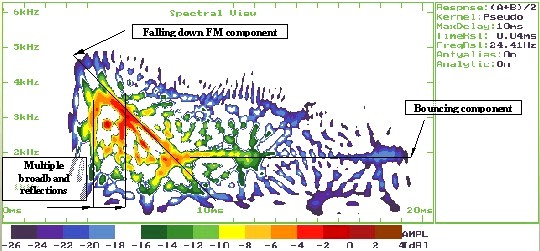




















 Scala media stimulation: A glass microelectrode is inserted into the scala media through the lateral wall or the basilar membrane (Figure 7). Constant current is injected into the scala media using the microelectrode. The tip diameter of the electrode is approximately 5 mm and the microelectrode is filled with 0.16 M, 1 M, or 3 M KCl. A Ag/AgCl wire is inserted into the neck muscles to serve as the current return electrode. The intensity of the currents could range from 1 to 50 mA peak-to-peak.
Scala media stimulation: A glass microelectrode is inserted into the scala media through the lateral wall or the basilar membrane (Figure 7). Constant current is injected into the scala media using the microelectrode. The tip diameter of the electrode is approximately 5 mm and the microelectrode is filled with 0.16 M, 1 M, or 3 M KCl. A Ag/AgCl wire is inserted into the neck muscles to serve as the current return electrode. The intensity of the currents could range from 1 to 50 mA peak-to-peak. Scala tympani stimulation: A platinum-iridium wire is usually used (50-75 mm in diameter) for electrical current stimulation. The electrode is placed into the scala tympani (Figure 8). For monopolar electrode configuration, the Ag/AgCl wire (serving as the return electrode) is inserted into the neck muscles. For bipolar electrode configuration, a second platinum-iridium wire is placed into the scala tympani (or scala vestibuli) as the return electrode. The intensity of the currents could be 10 to 50 mA rms.
Scala tympani stimulation: A platinum-iridium wire is usually used (50-75 mm in diameter) for electrical current stimulation. The electrode is placed into the scala tympani (Figure 8). For monopolar electrode configuration, the Ag/AgCl wire (serving as the return electrode) is inserted into the neck muscles. For bipolar electrode configuration, a second platinum-iridium wire is placed into the scala tympani (or scala vestibuli) as the return electrode. The intensity of the currents could be 10 to 50 mA rms. Extracochlear (round window) stimulation: The electric current is delivered to the scala tympani through a platinum-iridium electrode in the round window niche. The Ag/AgCl wire in the neck serves as the return electrode (Figure 9). The electric current level could be from 10 to 300 mA rms.
Extracochlear (round window) stimulation: The electric current is delivered to the scala tympani through a platinum-iridium electrode in the round window niche. The Ag/AgCl wire in the neck serves as the return electrode (Figure 9). The electric current level could be from 10 to 300 mA rms.








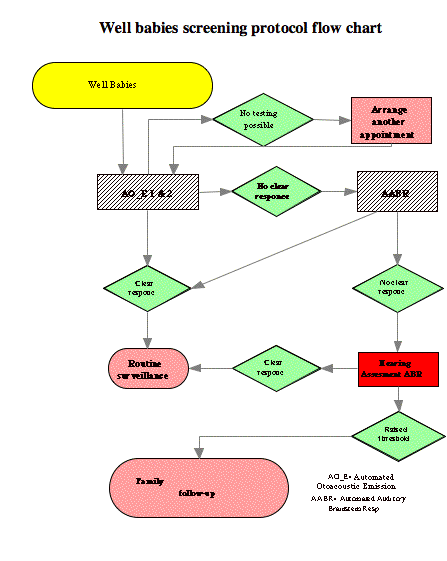
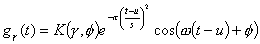 (1)
(1)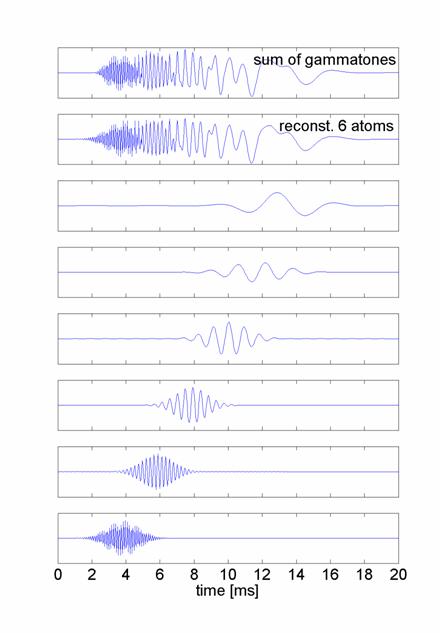
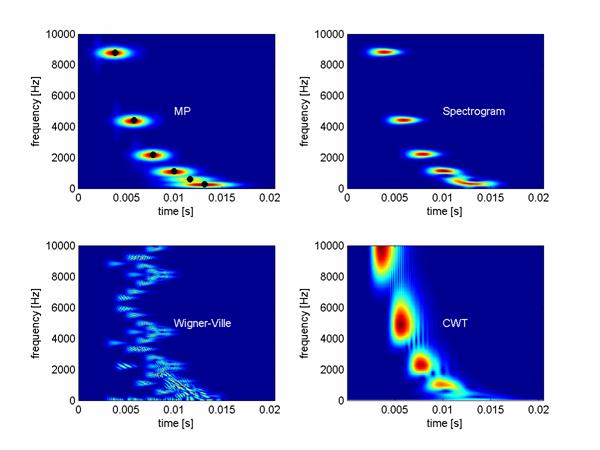

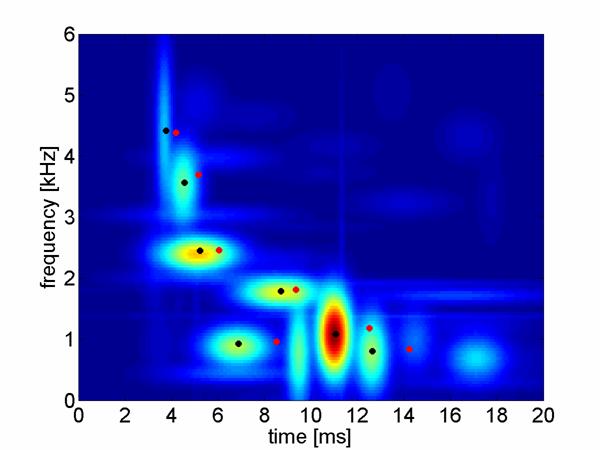
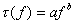 (2)
(2)
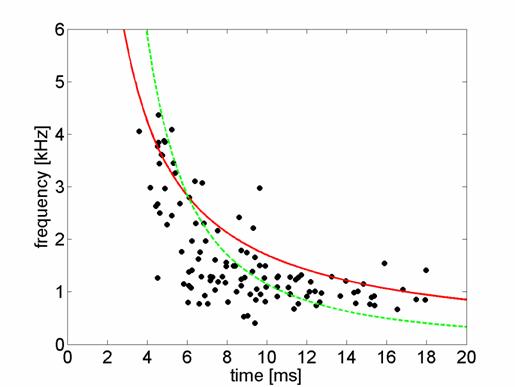
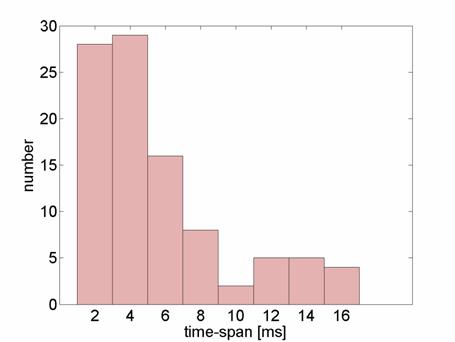
 Auditory Neuropathy : Introduction
Auditory Neuropathy : Introduction





 In two relatively recent papers, (Dhar & Shaffer, 2004; Shaffer & Dhar, 2006) have explored the possibility of improving the prediction of behavioral hearing thresholds from distortion product otoacoustic emission (DPOAE) level. DPOAEs are sounds generated in the cochlea (Kemp, 1979) that can be recorded in the ear canal using appropriate recording and analysis equipment. When a normally functioning cochlea is stimulated simultaneously with two pure tones, say at frequencies f1 and f2 (f1 < f2), the cochlea generates energy at various other frequencies related to those of the stimulus tones. The DPOAE produced at the frequency 2f1-f2 is commonly used for clinical purposes as it is easily recorded from human ears under certain stimulus conditions. DPOAEs at frequencies lower than those of the stimulus tones, such as that at the frequency 2f1-f2, can be called ÒapicalÓ DPOAEs as the tonotopic organization of the basilar membrane dictates that their characteristic frequency place lies apical to that of the stimulus tones.
In two relatively recent papers, (Dhar & Shaffer, 2004; Shaffer & Dhar, 2006) have explored the possibility of improving the prediction of behavioral hearing thresholds from distortion product otoacoustic emission (DPOAE) level. DPOAEs are sounds generated in the cochlea (Kemp, 1979) that can be recorded in the ear canal using appropriate recording and analysis equipment. When a normally functioning cochlea is stimulated simultaneously with two pure tones, say at frequencies f1 and f2 (f1 < f2), the cochlea generates energy at various other frequencies related to those of the stimulus tones. The DPOAE produced at the frequency 2f1-f2 is commonly used for clinical purposes as it is easily recorded from human ears under certain stimulus conditions. DPOAEs at frequencies lower than those of the stimulus tones, such as that at the frequency 2f1-f2, can be called ÒapicalÓ DPOAEs as the tonotopic organization of the basilar membrane dictates that their characteristic frequency place lies apical to that of the stimulus tones.











































 The
The 
 symbol indicate already presented material. The data are shown from more recent to older. Links will be inserted when the whole Portal material is transferred.
symbol indicate already presented material. The data are shown from more recent to older. Links will be inserted when the whole Portal material is transferred.
















